EULAR 2016:系统性红斑狼疮增加女性患宫颈癌的风险
2016-06-11 MedSci MedSci原创
卡罗琳斯卡医学院的Hjalmar Wadström博士和他的同事将研究结果在2016年欧洲风湿病年度会议(EULAR2016)上提出。 在谈到红斑狼疮时,大多数人都认为是系统性红斑狼疮(SLE),因为该病是最常见的疾病类型。系统性红斑狼疮是一种自身免疫性疾病,免疫系统攻击自身的组织和器官,受累部位包括皮肤、关节、大脑、肾脏和血管。根据狼疮研究所的数据显示,美国约有150名系统性红斑狼疮患者,其中超
卡罗琳斯卡医学院的Hjalmar Wadström博士和他的同事将研究结果在2016年欧洲风湿病年度会议(EULAR 2016)上提出。
在谈到红斑狼疮时,大多数人都认为是系统性红斑狼疮(SLE),因为该病是最常见的疾病类型。系统性红斑狼疮是一种自身免疫性疾病,免疫系统攻击自身的组织和器官,受累部位包括皮肤、关节、大脑、肾脏和血管。根据狼疮研究所的数据显示,美国约有150名系统性红斑狼疮患者,其中超过90%是年龄介于15至44岁之间的女性。
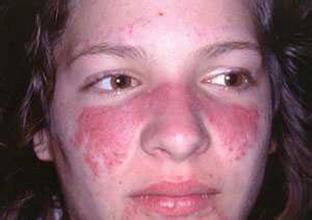
虽然系统性红斑狼疮的临床表现各不相同,但常见表现包括关节疼痛或肿胀、皮疹和溃疡、阳光敏感性、肌肉疼痛、发烧、疲劳和口腔溃疡等。对年轻女性而言,系统性红斑狼疮会增加她们发生心血管疾病如卒中和肾脏疾病的风险。
既往研究表明,自身免疫性疾病可能会增加女性患宫颈癌的风险,但Wadstrom博士及其同事指出,这样的证据是相互矛盾的。为了探究系统性红斑狼疮和宫颈癌之间的联系,研究人员对瑞典国家肿瘤患者登记数据、瑞典国家宫颈癌筛查数据等信息进行了分析。
通过使用这些数据,研究人员计算普通女性和系统性红斑狼疮女性患者在2006-2012年发生浸润性宫颈癌和宫颈发育不良的发生率。
研究人员发现,女性系统性红斑狼疮患者发生浸润性宫颈癌和宫颈发育不良的风险是普通女性的2倍。服用免疫抑制剂药物的SLE女性发生浸润性宫颈癌和宫颈发育不良风险最高。
在考虑了年龄、性别、教育、医疗保健、宝宝数目、婚姻状况、宫颈癌家族史和5年内宫颈癌筛查史等信息后,该结论依旧成立。研究人员指出,该研究结果强调SLE女性进行宫颈癌筛查的重要性,无论她们是否服用免疫抑制剂药物治疗,都应该进行常规宫颈癌筛查。系统性红斑狼疮是女性患宫颈癌的高危风险因素。
原始出处:
1.Lupus confirmed as risk factor for cervical cancer.EurekAlert.June 9, 2016.
2.Hongli Liu,et al. Meta-analysis of systemic lupus erythematosus and the risk of cervical neoplasia. Rheumatology.2010 August 12.
本网站所有内容来源注明为“梅斯医学”或“MedSci原创”的文字、图片和音视频资料,版权均属于梅斯医学所有。非经授权,任何媒体、网站或个人不得转载,授权转载时须注明来源为“梅斯医学”。其它来源的文章系转载文章,或“梅斯号”自媒体发布的文章,仅系出于传递更多信息之目的,本站仅负责审核内容合规,其内容不代表本站立场,本站不负责内容的准确性和版权。如果存在侵权、或不希望被转载的媒体或个人可与我们联系,我们将立即进行删除处理。
在此留言












#系统性#
32
继续学习
81
继续关注
66
#狼疮#
33
#宫颈#
30
#红斑#
32
#EULAR#
0