BJC:转移性结直肠癌患者原发肿瘤部位对贝伐单抗联合化疗疗效的影响
2018-11-30 MedSci MedSci原创
两项一线贝伐单抗临床试验结果明确了原发肿瘤位置在转移性结直肠癌(mCRC)中的预后价值。BJC近期发表了一篇文章,在回顾性亚组分析中进一步分析了贝伐单抗的预测效果。
两项一线贝伐单抗临床试验结果明确了原发肿瘤位置在转移性结直肠癌(mCRC)中的预后价值。BJC近期发表了一篇文章,在回顾性亚组分析中进一步分析了贝伐单抗的预测效果。
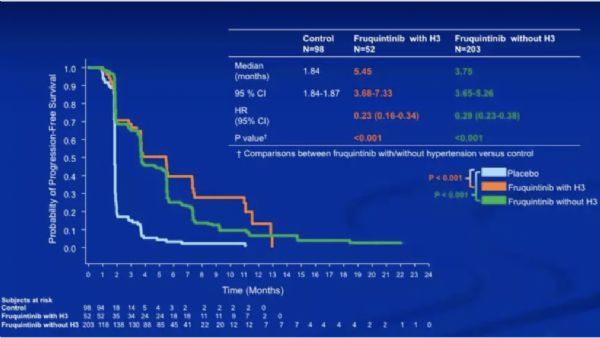
作者对两项贝伐单抗+化疗(CT)与单纯化疗比较治疗转移性结直肠癌的随机III期临床试验的患者进行了回顾性分析。研究结果表明,2290名患者中有1590名(27%右侧和73%左侧)明确原发肿瘤位置。在左侧原发肿瘤和右侧原发肿瘤患者中,贝伐单抗+ 化疗与单纯化疗相比均可以改善患者无进展生存情况。同样,右侧转移性结直肠癌患者中贝伐单抗+化疗与单纯化疗相比总体生存率得到改善,但无统计学意义。左侧转移性结直肠癌患者显着改善。
原始出处:
Fotios Loupakis, Herbert I. Hurwitz, et al. Impact of primary tumour location on efficacy of bevacizumab plus chemotherapy in metastatic colorectal cancer BJC. November 2018 doi: https://doi.org/10.1038/s41416-018-0304-6
本文系梅斯医学(MedSci)原创编译整理,转载需授权!
本网站所有内容来源注明为“梅斯医学”或“MedSci原创”的文字、图片和音视频资料,版权均属于梅斯医学所有。非经授权,任何媒体、网站或个人不得转载,授权转载时须注明来源为“梅斯医学”。其它来源的文章系转载文章,或“梅斯号”自媒体发布的文章,仅系出于传递更多信息之目的,本站仅负责审核内容合规,其内容不代表本站立场,本站不负责内容的准确性和版权。如果存在侵权、或不希望被转载的媒体或个人可与我们联系,我们将立即进行删除处理。
在此留言












学习了,谢谢作者分享!
65
#原发肿瘤#
38
#转移性#
37
#联合化疗#
35
#结直肠#
28
#贝伐#
24
谢谢梅斯提供这么好的信息,学到很多
35