《中国巴雷特食管及其早期腺癌筛查与诊治共识》解读
2017-09-15 张澍田 中华医学信息导报
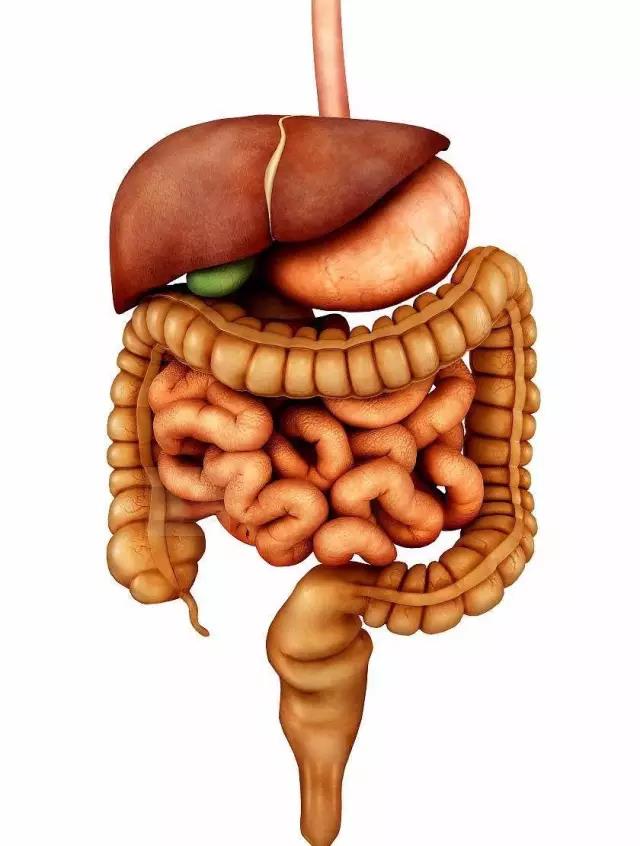
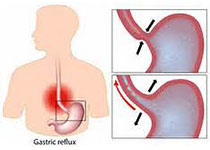
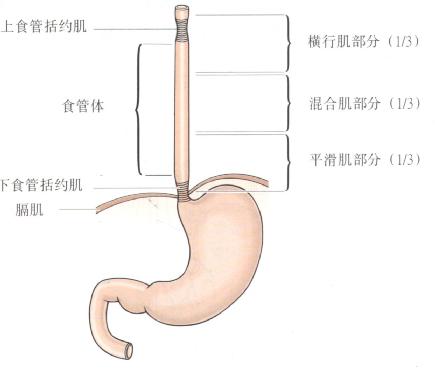
虽然我国食管癌的组织类型以食管鳞癌为主,但是随着世界范围内胃食管反流病的增加,我国巴雷特食管(Barrett's esophagus)/食管下段柱状上皮化生和食管腺癌的发病率也在增加,同样威胁着人们的生命。有报道显示,在食管腺癌中有80%与巴雷特食管密切相关,而我国巴雷特食管的癌变率和西方国家相近,为61%左右。

本网站所有内容来源注明为“梅斯医学”或“MedSci原创”的文字、图片和音视频资料,版权均属于梅斯医学所有。非经授权,任何媒体、网站或个人不得转载,授权转载时须注明来源为“梅斯医学”。其它来源的文章系转载文章,或“梅斯号”自媒体发布的文章,仅系出于传递更多信息之目的,本站仅负责审核内容合规,其内容不代表本站立场,本站不负责内容的准确性和版权。如果存在侵权、或不希望被转载的媒体或个人可与我们联系,我们将立即进行删除处理。
在此留言









#筛查与诊治#
28
学习了
73
非常好.学习了.谢谢
64
学习了
66
学习了谢谢分享
71
#巴雷特食管#
39
#食管#
31
文章很好.赞赞赞
58
这个要好好学习才行
27