【所属科室】
泌尿外科
【基本资料】
女性,66岁。
【主诉】
右侧腰痛伴间断性肉眼血尿10余天,疼痛为阵发性,可自行缓解,疼痛发作时有发热
【查体】
36.5度,余无明显异常。
【辅助检查】
B超:右肾占位
【影像图片】
【讨论】
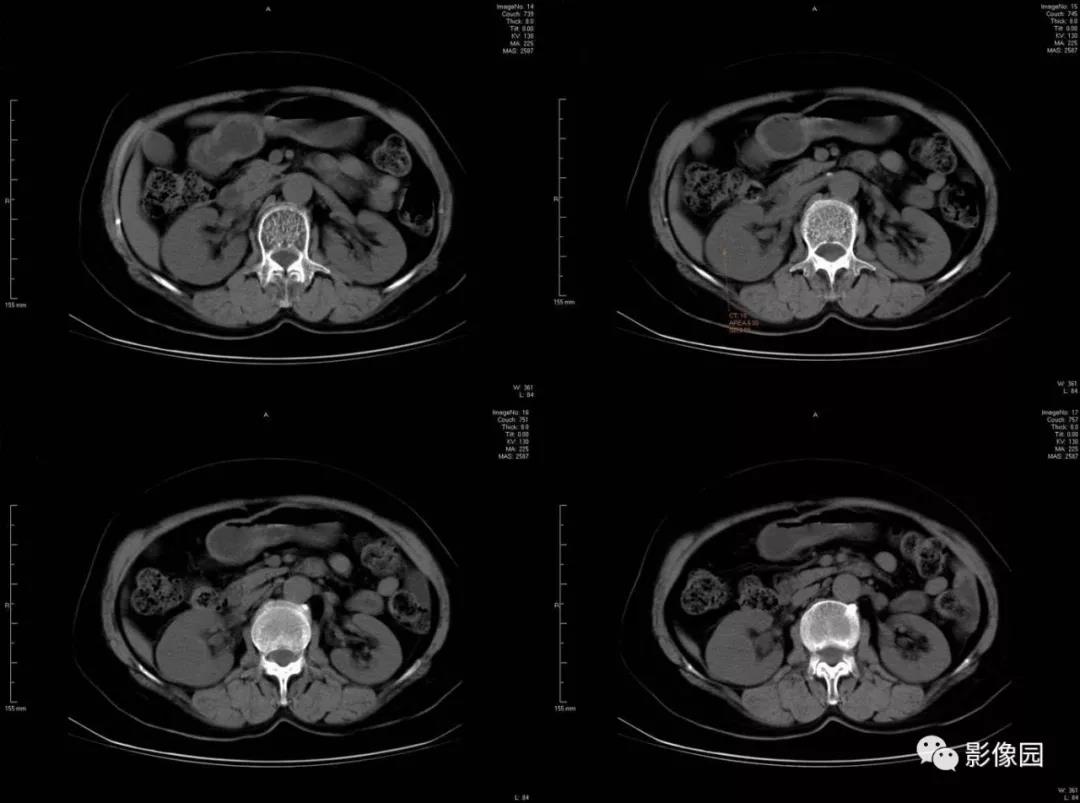
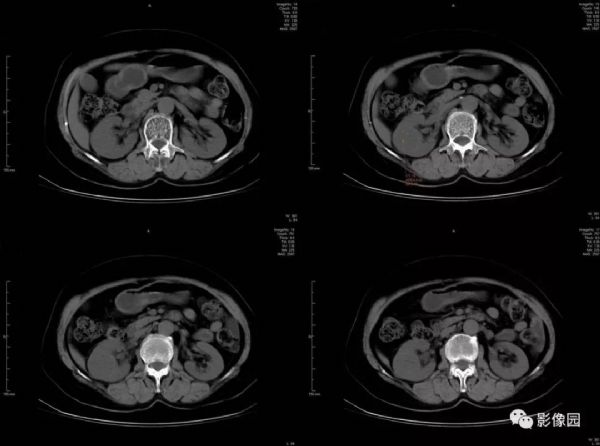
评论:平扫右肾实质内可见一类圆形稍低密度影,密度均匀,与肾组织边界欠清。增强扫描后肾实质明显强化,肿块边缘强化,囊壁稍显增厚。尿路造影片示右侧肾盂肾盏受压改变。
【病理结果】
手术病理:右肾炎性假瘤(直径3cm),周围肾间质慢性炎症
【病例小结】
肾脏炎性假瘤可发生于任何年龄,以40岁以下者居多,男女发病无明显差别。患者多有低热、腰痛、肾区不适或有疼痛、扣痛等,部分病人有血尿、脓尿,通常无尿路刺激症状。本病的病程可以自数天到数年,预后良好。1、CT表现:
1)平扫肿块呈类圆形或不规则形,直径一般为2~5mm,密度与肾实质密度大致相似,边界不清,CT值20~40HU。2)增强扫描实质期病灶实质部分轻度强化,边缘部分可呈较明显环形强化。3)患侧肾筋膜增厚,可有肾周模糊。2、与肾癌鉴别:早期肾癌(尤其 <3 cm 的小肾癌) ,因肾细胞癌大多血供丰富, 增强扫描的皮质期明显强化,实质期瘤体强化迅速减弱。而炎性假瘤血供较少。3、本例特点:1)平扫病灶略低于肾实质
2)增强边界清楚,周边略呈环形强化。病灶为类圆形,实质部分密度均匀,强化不明显。
3)右肾前筋膜稍增厚
版权声明:
本网站所有内容来源注明为“梅斯医学”或“MedSci原创”的文字、图片和音视频资料,版权均属于梅斯医学所有。非经授权,任何媒体、网站或个人不得转载,授权转载时须注明来源为“梅斯医学”。其它来源的文章系转载文章,或“梅斯号”自媒体发布的文章,仅系出于传递更多信息之目的,本站仅负责审核内容合规,其内容不代表本站立场,本站不负责内容的准确性和版权。如果存在侵权、或不希望被转载的媒体或个人可与我们联系,我们将立即进行删除处理。
在此留言
本网站所有内容来源注明为“梅斯医学”或“MedSci原创”的文字、图片和音视频资料,版权均属于梅斯医学所有。非经授权,任何媒体、网站或个人不得转载,授权转载时须注明来源为“梅斯医学”。其它来源的文章系转载文章,或“梅斯号”自媒体发布的文章,仅系出于传递更多信息之目的,本站仅负责审核内容合规,其内容不代表本站立场,本站不负责内容的准确性和版权。如果存在侵权、或不希望被转载的媒体或个人可与我们联系,我们将立即进行删除处理。
在此留言










#间断性#
28
#间断#
32
#肉眼血尿#
37
#血尿#
31