J Gastroenterology:日本炎症性肠病患者中动静脉血栓栓塞导致死亡的危险因素分析
2021-11-16 MedSci原创 MedSci原创
炎性肠病又称炎症性肠病(IBD),为累及回肠、直肠、结肠的一种特发性肠道炎症性疾病。
炎症性肠病 (IBD) 是一种慢性复发性的累及肠道和全身的炎症性疾病,它有两种主要的表型:溃疡性结肠炎 (UC) 和克罗恩病 (CD)。血栓栓塞(TE)是一种严重的肠外表现,事实上,来自西方国家的大规模队列研究表明,IBD 患者静脉血栓栓塞 (VTE) 的发生率是非 IBD患者的两到三倍。近年来,一些研究报告表明,与非 IBD 患者相比,IBD 患者发生动脉血栓栓塞 (ATE) 的风险明显增加,包括缺血性心脏病 (IHD) 和脑血管疾病 (CVD)的风险均明显增加。值得注意的是,ATE 和 VTE 在临床实践中被视为危及IBD患者生命的并发症,因此,可能需要侵入性治疗(进入重症监护室、导管干预和手术)。因此,本项研究旨在揭示日本 IBD 患者 TE 的死亡率和危险因素。
研究人员为此从日本的32个医疗机构中收集了过去10年间所有IBD患者的严重TE和TE 相关死亡病例的资料。同时回顾性收集IBD患者发生TE时的临床特征、实验室数据、治疗状态和疾病进展情况,并比较有无严重TE患者和TE相关死亡患者的数据。

研究结果显示在31940名IBD患者中,TE的发生率为1.89%。在IBD和TE合并IBD患者中,严重TE和TE相关死亡率的频率分别为10.7%和1.0%。严重 ATE 和 ATE 相关死亡的唯一危险因素是缺血性心脏病。严重VTE和VTE相关死亡的独立危险因素是年龄(≤45 岁)、VTE 部位和疾病严重程度,抗TNF治疗是潜在的负面危险因素。严重 VTE 患者发生持续性 VTE 和后遗症的风险很高。
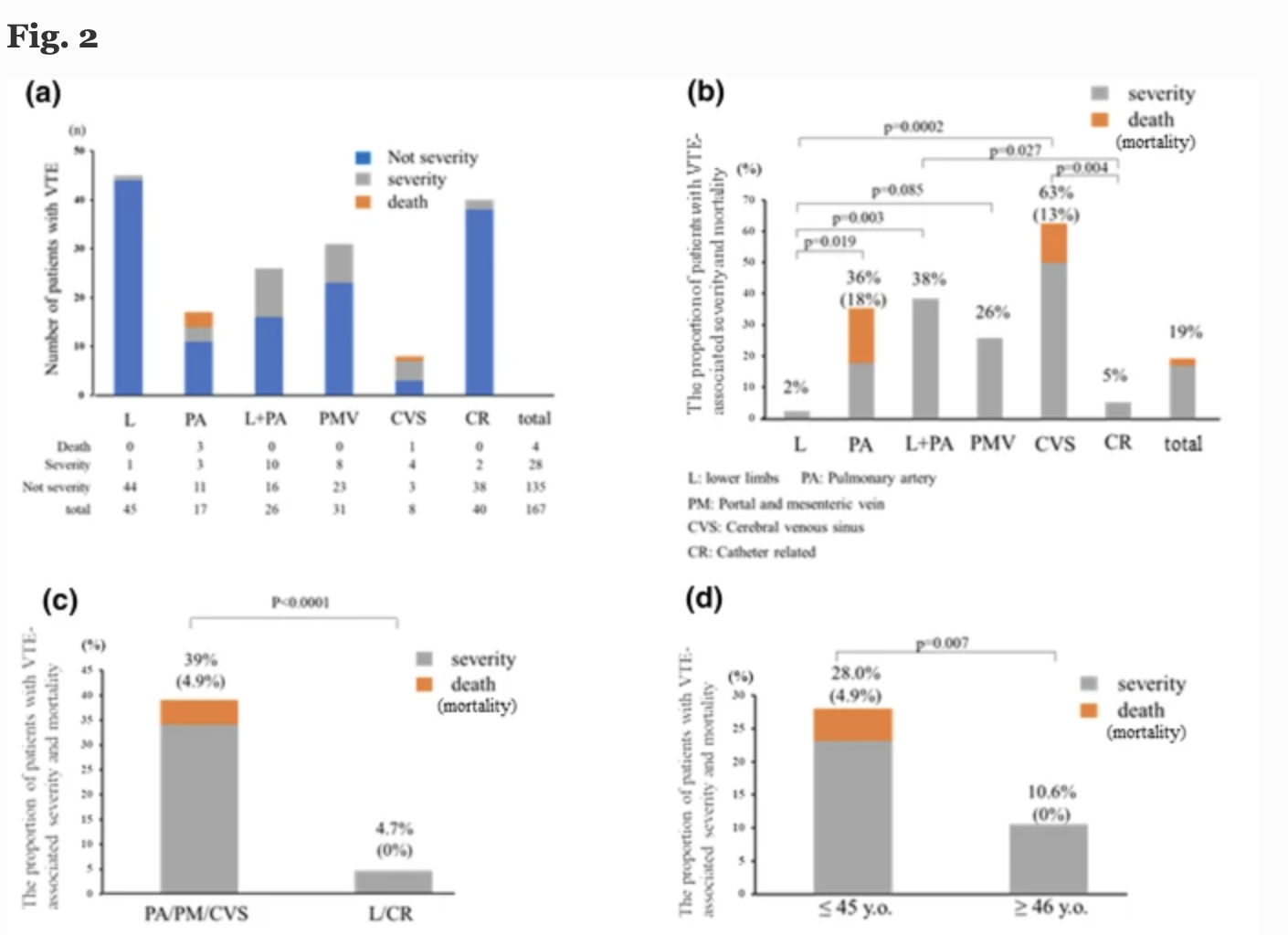
本项研究证实,亚洲IBD患者的ATE发生率显著低于西方国家,而且严重VTE的发生率为 20%,这些病例往往表现出持续性 VTE、发展后遗症和死亡的高风险。因此,临床上迫切需要针对亚洲人群 IBD 相关 TE 的适当风险分类系统、筛查和预防策略。
原始出处:
Katsuyoshi Ando. Et al. A nationwide survey concerning the mortality and risk of progressing severity due to arterial and venous thromboembolism in inflammatory bowel disease in Japan. Journal of Gastroenterology.2021.
本网站所有内容来源注明为“梅斯医学”或“MedSci原创”的文字、图片和音视频资料,版权均属于梅斯医学所有。非经授权,任何媒体、网站或个人不得转载,授权转载时须注明来源为“梅斯医学”。其它来源的文章系转载文章,或“梅斯号”自媒体发布的文章,仅系出于传递更多信息之目的,本站仅负责审核内容合规,其内容不代表本站立场,本站不负责内容的准确性和版权。如果存在侵权、或不希望被转载的媒体或个人可与我们联系,我们将立即进行删除处理。
在此留言










#GAS#
43
#静脉#
48
#AST#
36
#静脉血#
42
#Gastroenterol#
32
#日本#
37
#Gastroenterology#
33
#炎症性#
34
#炎症性肠病患者#
42
有年龄为>18岁的1型糖尿病患者接受HCLS
177