Ann Rheum Dis:Meta分析揭示不同抗风湿药物的心血管事件风险差异
2015-02-18 梁怀彬 译 MedSci原创
研究者为了明确心血管事件(CVEs)和抗风湿药物的关系,进行了一项系统评价和Meta分析。该研究中使用抗风湿治疗的患者人群为类风湿关节炎(RA)、银屑病关节炎(PsA)/银屑病(Pso)患者。研究者系统性检索了MEDLINE,EMBASE,Cochrane databases里1960到2012年12月份发表的随机对照研究和相关的重要会议记录(2010-2012,文献需包含确定的CVEs信息和使用
研究者系统性检索了MEDLINE,EMBASE,Cochrane databases里1960到2012年12月份发表的随机对照研究和相关的重要会议记录(2010-2012,文献需包含确定的CVEs信息和使用抗风湿药物情况。研究者对提取出的数据进行随机效应模型Meta分析。
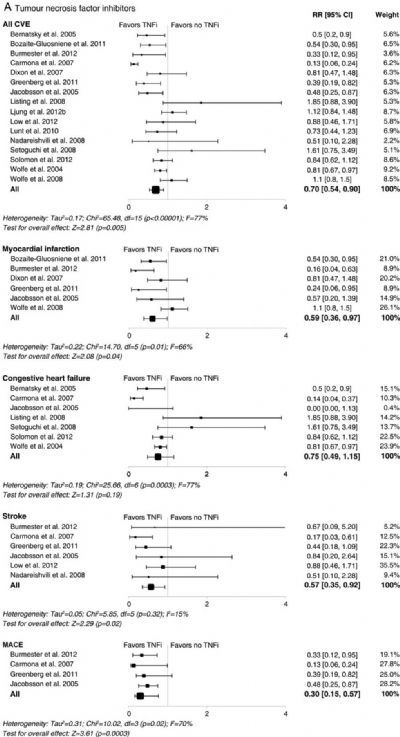
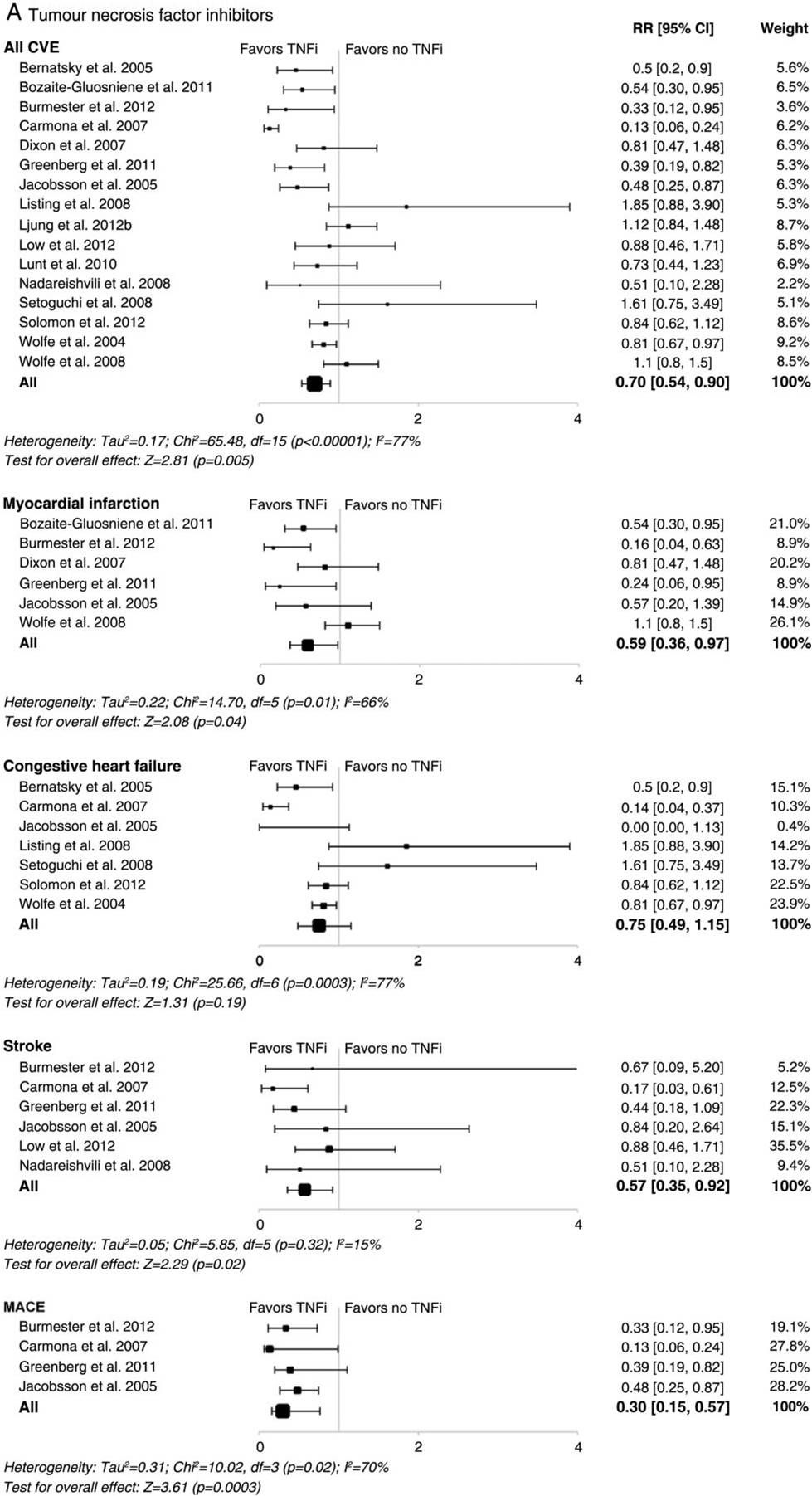
在上述文献库中研究者检索到2630篇文献,34个研究通过了筛选,其中28个研究的研究群体是RA,6个是Psa/Pso。在RA患者当中,TNF抑制剂、甲氨蝶呤可降低CVEs风险。相关危险比RR分别为为0.70(95% CI 0.54 to 0.90; p=0.005)和0.72(95% CI 0.57 to 0.91; p=0.007),非甾体抗炎药增加CVEs风险,RR为1.18(95% CI 1.01 to 1.38; p=0.04),这其中导致这种结果一直以来尤其以罗非昔布为典型。糖皮质激素也增加CVEs事件发生风险,RR为1.47(95% CI 1.34 to 1.60; p<0.001)。在Psa/Pso患者当中系统性治疗方案降低CVEs风险,RR为0.75(95% CI 0.63 to 0.91; p=0.003)。
研究者得出结论:RA患者治疗中,TNF抑制剂和甲氨蝶呤会降低心血管事件发生风险,非甾体抗炎药和糖皮质激素会增加心血管风险。靶向抗炎药物TNF抑制剂和甲氨蝶呤在类风湿患者中可能有着积极的心血管保护效应。有限的证据表明系统性治疗方案降低银屑病/银屑病关节炎患者心血管事件发生风险。
本网站所有内容来源注明为“梅斯医学”或“MedSci原创”的文字、图片和音视频资料,版权均属于梅斯医学所有。非经授权,任何媒体、网站或个人不得转载,授权转载时须注明来源为“梅斯医学”。其它来源的文章系转载文章,或“梅斯号”自媒体发布的文章,仅系出于传递更多信息之目的,本站仅负责审核内容合规,其内容不代表本站立场,本站不负责内容的准确性和版权。如果存在侵权、或不希望被转载的媒体或个人可与我们联系,我们将立即进行删除处理。
在此留言








#Dis#
41
#MET#
32
#血管事件#
39
#Meta#
38
#心血管事件风险#
23