EASL 2014:白蛋白输注不改善合并细菌感染的肝硬化患者生存
2014-04-14 佚名 dxy
白蛋白输注能有效提高合并自发性腹膜炎(SBP)的肝硬化患者的生存率,但它对合并细菌感染(不包括自发性腹膜炎)的肝硬化患者的作用尚未明确。法国贝桑松明热斯医院Thevenot等对此进行了一项多中心随机对照试验研究,其结果在2014年4月9日至4月13日的EASL2014会上公布。 研究共纳入191名肝硬化患者(涉及25个研究中心,男性占68%,年龄平均55岁,92%为酒精性肝硬化),纳入标准为Ch
白蛋白输注能有效提高合并自发性腹膜炎(SBP)的肝硬化患者的生存率,但它对合并细菌感染(不包括自发性腹膜炎)的肝硬化患者的作用尚未明确。法国贝桑松明热斯医院Thevenot等对此进行了一项多中心随机对照试验研究,其结果在2014年4月9日至4月13日的EASL2014会上公布。
研究共纳入191名肝硬化患者(涉及25个研究中心,男性占68%,年龄平均55岁,92%为酒精性肝硬化),纳入标准为Child-Pugh分级得分>8分者且伴发脓毒症(除了SBP)。患者随机分为A、B两组,A组患者(共95例)接受抗生素及白蛋白输注治疗(第一天输注量为1.5g/kg,第三天输注量为1g/kg);B组患者(共96例)则只接受抗生素治疗。主要观察指标是三个月后两组患者肾功能衰竭(血肌酐水平上升50%,达15mg/L以上)的发生率。
结果表明,两组患者的年龄、性别、Child-Pugh评分、重度酒精性肝炎比例、感染类型(肺炎占33.3%,重症败血症占13.3%)、血钠水平和血肌酐水平差异无统计学意义。A组患者同时伴有腹水的比例高于B组(75.8% VS 59.6%7)。47名患者在观察期内死亡(A组27名,B组20名,两组的三月生存率分别为70.2%和78.3%),其主要死亡原因见表1。
表1 两组患者的死亡原因统计
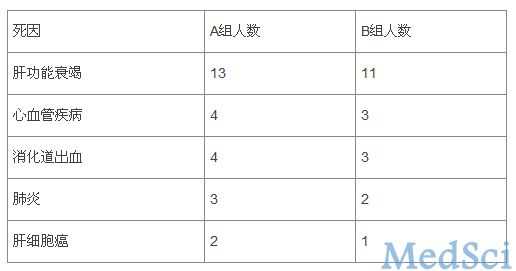
13.9%的患者(共25名)发展为肾功能衰竭,A组与B组肾衰发生率分别为14.3%和13.5%,平均延时分别为29.0±21.8天和11.7±9.1天。肾衰患者的死亡率明显升高(60% VS 11.8%)。另外,9名患者发展为肺充血,其中3名患者死亡。
研究结果显示,白蛋白输注对于合并细菌感染(不包括自发性腹膜炎)的肝硬化患者而言,不能改善其肾功能、亦不能提高其三月生存率。
本网站所有内容来源注明为“梅斯医学”或“MedSci原创”的文字、图片和音视频资料,版权均属于梅斯医学所有。非经授权,任何媒体、网站或个人不得转载,授权转载时须注明来源为“梅斯医学”。其它来源的文章系转载文章,或“梅斯号”自媒体发布的文章,仅系出于传递更多信息之目的,本站仅负责审核内容合规,其内容不代表本站立场,本站不负责内容的准确性和版权。如果存在侵权、或不希望被转载的媒体或个人可与我们联系,我们将立即进行删除处理。
在此留言








#患者生存#
26
#细菌感染#
26
#白蛋白#
35
#EASL#
33
#ASL#
23