Movement disorders:帕金森病:黑质中的铁沉积,如何随时间变化?
2022-07-01 Freeman MedSci原创
在开始使用多巴胺能药物治疗之前,黑质铁较低,然后在整个疾病过程中不断增加,直到晚期达到平稳
帕金森病(PD)的病理特征是基底神经节黑质(SN)旁的多巴胺神经元的损失。自1987年Dexter等人首次报道11名死后PD患者的SN中铁含量增加以来,一些死后研究显示PD患者的黑质铁浓度更高。此外,临床前研究的结果表明,细胞内铁过量与PD的氧化应激、细胞功能障碍和神经元死亡有关,可能在PD发病机制中起作用。

图1: 论文封面图
因此,有人提出用铁螯合疗法来改变疾病过程。然而,目前还不清楚黑质铁是否在PD诊断前就已积累,以及它在疾病发展过程中是如何演变的。此外,铁是否是疾病本身的后果和/或受到医疗干预(如抗帕金森病药物)的影响,也是未知的。
最近核磁共振技术的进步使人类大脑铁含量的体内评估成为可能。20 敏感性MRI已被证明与死后组织学测量的铁有很好的相关性。许多先前的研究,包括我们小组的研究,已经利用表观横向弛豫率(R2*)和较新的定量易感性图谱(QSM)来了解铁在PD中的作用。
与早期的病理报告相一致,许多这些体内MRI研究表明PD患者的黑质铁含量较高。有趣的是,无论是尸检报告还是我们最近的MRI研究,都没有在早期PD患者中发现较高的黑质铁。此外,我们发现这些早期参与者的黑质铁在18个月内没有明显的变化。
值得注意的是,除了在引入左旋多巴之前的一项尸检研究外,所有调查黑质铁的尸检和MRI研究都来自正在服用抗帕金森药物的PD患者。此外,我们以前的研究表明,黑质铁含量的进展是非线性和阶段性的。 然而,目前还不清楚铁的积累是否只是PD进展的结果,还是与常用药物有关。
目前的研究采用了最先进的脑部易感性核磁共振成像分析,以调查新诊断的无药(PDDN)和药物治疗(PDDT)PD患者的脑部铁沉积。
藉此,宾夕法利亚州立大学的Guangwei Du等人测试了两个假设:(1)与对照组或病程较长的PDDT PD患者相比,新诊断的PDDN PD患者的黑质铁含量并不明显较高;
(2)在引入抗帕金森药物治疗后发生的铁沉积增加可能与所服用的药物有关。

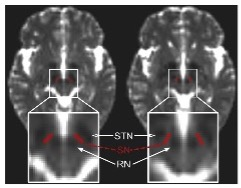
图2:论文结果图
敏感性磁共振成像数据来自79名对照组和18名无药(PDDN)和87名药物治疗(PDDT)PD患者。基底神经节和小脑结构中的区域性脑铁是用定量易感性图谱来估计的。对PDDN和PDDT亚组之间的脑铁进行了比较,亚组的定义是疾病持续时间(早期[PDE,<2年],中期[PDM,2-6年],和后期[PDL,>6年])。使用回归分析探讨了与病程和抗帕金森病药物类型的关系。
与对照组相比,PDDN在黑质(P = 0.018)、尾状核(P = 0.038)和苍白球(P = 0.01)中的铁含量较低,但在putamen或红核中却没有。
相反,与对照组或PDDN相比,PDDT在黑区的铁含量较高(P < 0.001),但在其他区域没有。黑质中的铁随着病程的延长而增加(PDE>PDDN[P=0.001],PDM>PDE[P=0.045]),但PDM与PDL相比(P=0.226)。使用左旋多巴与较高的(P = 0.013)黑质铁有关,而较低的黑质铁则与使用西格列汀有关(P = 0.030)。
该研究的重要意义在于发现了:在开始使用多巴胺能药物治疗之前,黑质铁较低,然后在整个疾病过程中不断增加,直到晚期达到平稳,这表明铁的增加可能不是一个病因学因素。有趣的是,PD药物可能与铁积累有不同的关联,需要进一步调查。
原文出处:
Du G, Wang E, Sica C, et al. Dynamics of Nigral Iron Accumulation in Parkinson’s Disease: From Diagnosis to Late Stage. _Movement Disorders_. Published online May 25, 2022:mds.29062. doi:[10.1002/mds.29062](https://doi.org/10.1002/mds.29062)
本网站所有内容来源注明为“梅斯医学”或“MedSci原创”的文字、图片和音视频资料,版权均属于梅斯医学所有。非经授权,任何媒体、网站或个人不得转载,授权转载时须注明来源为“梅斯医学”。其它来源的文章系转载文章,或“梅斯号”自媒体发布的文章,仅系出于传递更多信息之目的,本站仅负责审核内容合规,其内容不代表本站立场,本站不负责内容的准确性和版权。如果存在侵权、或不希望被转载的媒体或个人可与我们联系,我们将立即进行删除处理。
在此留言

















#铁沉积#
45
#ERS#
33
#disorders#
52
#Dis#
44
#disorder#
48
#Disord#
37