Movement disorders:帕金森患者,糖尿病可加速其进展
2022-06-26 Freeman MedSci原创
T2DM与帕金森病的疾病进展速度有关,突出了这两种疾病之间的互动。
帕金森病(PD)影响着全世界600万人,而且随着人口老龄化的到来,其发病率预计会增加。尽管衰老无疑是最重要的风险因素,但有证据表明2型糖尿病(T2DM)是一个适度的风险因素。此外,越来越多的证据表明,这些疾病有共同的生物机制,并有共同的遗传联系,突出了胰岛素信号传导失调可能是导致这些疾病之间关联的一个聚合途径。
 图1: 论文封面图
图1: 论文封面图
胰岛素受体在整个大脑中广泛表达,在PD、多系统萎缩和阿尔茨海默病(AD)的尸检研究中发现了神经元胰岛素信号传导缺陷的证据。胰岛素信号传导的缺陷导致主要下游途径的功能障碍,包括Akt和丝裂原活化蛋白激酶途径。这些途径反过来又调节着维持神经元生存所必需的各种过程,包括自噬、蛋白质合成、炎症、神经细胞代谢以及多巴胺的合成和清除,所有这些在PD中都会被破坏,因此可能被合并的T2DM所加剧/触发。与没有T2DM的患者相比,PD+T2DM患者在尾状体和腹侧纹状体表现出更严重的多巴胺能耗竭,以及更多的额颞叶皮质萎缩,进一步支持胰岛素抵抗对神经变性的影响。
除了对PD风险的影响外,少数研究还评估了T2DM对疾病进展的影响,认为与没有T2DM的PD患者相比,合并T2DM可能与运动和认知能力的快速下降有关。然而,这些研究的普遍性由于所包括的患者数量较少而受到限制。
藉此,英国Francis Crick Institute的Dilan Athauda等人,利用跟踪帕金森病队列这一大型的PD长期观察研究,目的是首先评估最近被诊断为PD的患者中合并T2DM与PD严重程度的关系,其次是确定T2DM是否对疾病进展产生负面影响。
他们分析了跟踪帕金森病研究的数据,通过比较评估一系列运动和非运动症状的症状严重程度,研究合并T2DM对PD进展和生活质量的影响。
他们确定了167名(8.7%)PD和T2DM(PD+T2DM)患者和1763名(91.3%)无T2DM(PD)的PD患者。
在控制了混杂因素后,T2DM患者有更严重的运动症状,根据运动障碍协会统一帕金森病评定量表第三部分评估(25.8 [0.9] vs. 22.5 [0.3] P = 0.002),以及非运动症状,根据非运动症状量表总数评估(38. 4 [2.5] vs. 31.8 [0.7] P <0.001),并且明显更有可能报告丧失独立性(几率比,2.08;95%置信区间[CI]:1.34-3.25;P = 0.001)和抑郁症(几率比,1.62;CI:1.10-2.39;P = 0.015)。
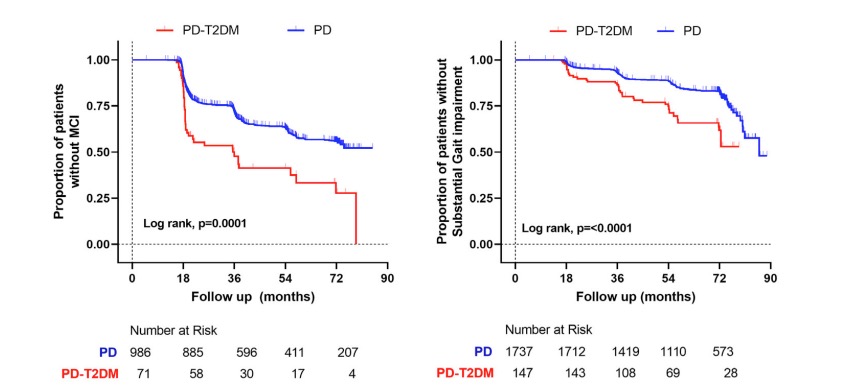 图2:论文结果图
图2:论文结果图
此外,随着时间的推移,与PD组相比,T2DM患者的运动症状进展明显加快(P = 0.012),情绪症状恶化(P = 0.041),并且更有可能出现实质性步态障碍(危险比,1.55;CI:1.07-2.23;P = 0.020)和轻度认知障碍(危险比,1.7;CI:1.24-2.51;P = 0.002)。
该研究的重要意义在于发现了:T2DM与帕金森病的疾病进展速度有关,突出了这两种疾病之间的互动。因为它是一种潜在的可改变的代谢状态,有多个外周和中枢的干预目标,它可能是缓解帕金森病症状和延缓残疾和痴呆进展的目标。
原文出处:
Athauda D, Evans J, Wernick A, et al. The Impact of Type 2 Diabetes in Parkinson’s Disease. _Movement Disorders_. Published online June 14, 2022:mds.29122. doi:[10.1002/mds.29122](https://doi.org/10.1002/mds.29122)
本网站所有内容来源注明为“梅斯医学”或“MedSci原创”的文字、图片和音视频资料,版权均属于梅斯医学所有。非经授权,任何媒体、网站或个人不得转载,授权转载时须注明来源为“梅斯医学”。其它来源的文章系转载文章,或“梅斯号”自媒体发布的文章,仅系出于传递更多信息之目的,本站仅负责审核内容合规,其内容不代表本站立场,本站不负责内容的准确性和版权。如果存在侵权、或不希望被转载的媒体或个人可与我们联系,我们将立即进行删除处理。
在此留言


















#disorder#
55
#Disord#
37
#disorders#
40
#ERS#
31
学习了,多谢分享
30
#Dis#
25