NEJM:Nivolumab辅助治疗方案用于晚期食管或胃食管交界癌患者III期临床研究获得成功
2021-04-04 MedSci原创 MedSci原创
对于需接受新辅助放化疗的食管癌或胃食管交界癌患者,nivolumab辅助治疗方案在无病生存期方面显著优于安慰剂

食道癌是全球第七大常见肿瘤,每年有超过50万人死亡。食管鳞状细胞癌,是食道癌最常见的组织学类型,近年来西方国家食管和胃食管交界癌的发病率呈现上升趋势。新辅助化疗联合手术是局部晚期食管或胃食管交界癌患者的标准治疗手段,但患者复发风险较高,70-75%病理学未完全应答患者治疗后复发,而淋巴结阳性患者的预后甚至更差。故需要开发新的局部晚期食管或胃食管交界癌患者的辅助化疗方案。

Checkmate577,一项全球、随机、双盲、安慰剂对照的3期试验,评估免疫检查点抑制剂Nivolumab作为食管或胃食管交界癌患者术后辅助治疗的可行性。新辅助放化疗并且残余病变切除(R0)的II或III期食管或胃食管交界癌成人患者参与研究,随机接受nivolumab治疗(初始剂量为每2周240mg,共16周,随后剂量为每4周480mg)或安慰剂。试验干预期最长为1年,主要终点是无病生存率。
研究平均随访24.4个月。Nivolumab治疗组532名患者的中位无病生存期为22.4个月,而安慰剂组262名患者的中位无病生存期为11.0个月(疾病复发或死亡的危险比=0.69)。Nivolumab在多个预先指定的亚组中显示出优势。Nivolumab组532名患者中有71名(13%)出现3级或4级不良事件,而安慰剂组260名患者中有15名(6%)。9%的Nivolumab组患者和3%的安慰剂组患者因治疗导致的不良事件停药。
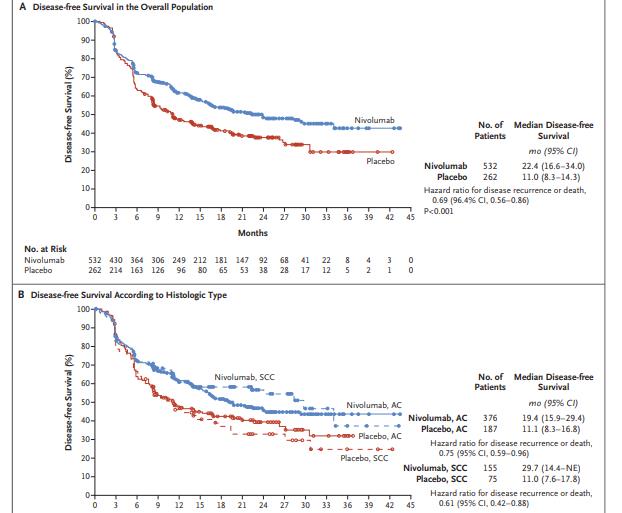
组间无病生存期差异
研究认为,对于需接受新辅助放化疗的食管癌或胃食管交界癌患者,nivolumab辅助治疗方案在无病生存期方面显著优于安慰剂。
原始出处:
Ronan J. Kelly et al. Adjuvant Nivolumab in Resected Esophageal or Gastroesophageal Junction Cancer. N Engl J Med, April 1, 2021.
本网站所有内容来源注明为“梅斯医学”或“MedSci原创”的文字、图片和音视频资料,版权均属于梅斯医学所有。非经授权,任何媒体、网站或个人不得转载,授权转载时须注明来源为“梅斯医学”。其它来源的文章系转载文章,或“梅斯号”自媒体发布的文章,仅系出于传递更多信息之目的,本站仅负责审核内容合规,其内容不代表本站立场,本站不负责内容的准确性和版权。如果存在侵权、或不希望被转载的媒体或个人可与我们联系,我们将立即进行删除处理。
在此留言










#NIV#
37
#III#
34
#III期临床研究#
38
#治疗方案#
28
学习的
60
#胃食管#
24
#mAb#
26
#I期临床#
32
#II期临床研究#
0
#食管#
26