Movement disorders:MRI新指标可有效鉴别帕金森和进行性核上麻痹
2022-06-15 Freeman MedSci原创
自动化的、经过验证的、可推广的磁共振生物标志物来区分PSP-P和PD
进行性核上性麻痹-帕金森病(PSP-P)和帕金森病(PD)之间的临床鉴别诊断可能具有挑战性,特别是在疾病发生后的头几年。PSP-P患者的临床表现主要是帕金森症,可以是不对称的,对左旋多巴有反应,与PD非常相似。PSP的唯一临床表现是眼球运动功能障碍,但核上垂直凝视麻痹可能在发病后19年才出现,因此诊断有时很困难。

图1: 论文封面图
迄今为止,一些影像学生物标志物已被证明有助于区分PSP和PD,而磁共振帕金森指数(MRPI)是最强大和最有力的标志之一。然而,这些影像学生物标志物大部分对PSP-理查德森综合征(PSP-RS)的诊断准确性很高,但未能准确区分PSP-P和PD患者,可能是因为这种较轻的PSP亚型的脑萎缩程度较低。
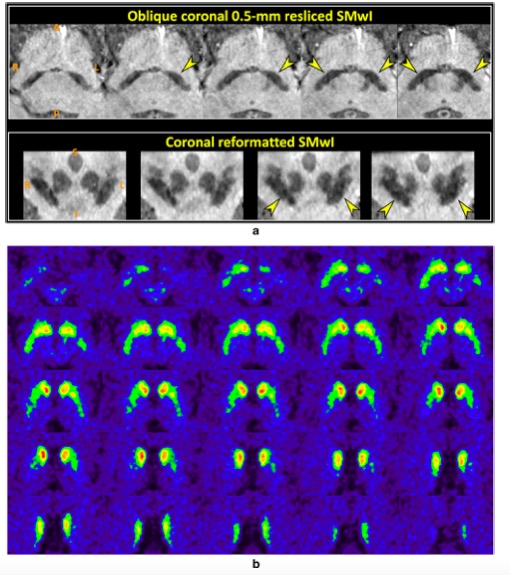
最近开发了新版本的MRPI(称为MRPI 2.0),以克服这一局限。除了MRPI测量的脑干结构(中脑、脑桥、小脑中段和上段)外,MRPI 2.0.还包括测量第三脑室(3 V)的宽度,这种脑结构在PSP患者中普遍增大,但在PD患者中却不存在。
初步结果显示,MRPI 2.0.能准确区分PSP-P患者和PD患者,但这一发现在最近的单中心研究中没有得到证实,该生物标志物区分PSP-P和PD的准确性较低,可能是由于手工测量的变异性和样本量小,因此提示需要自动计算MRPI 2.0.,并在较大的国际队列中进行验证性研究。
藉此,意大利University Magna Graecia的Andrea Quattrone等人,开发一种全自动的算法来计算MRPI 2.0.,并验证自动MRPI 2.0.在区分PSP-P患者和PD患者以及来自不同地区的两个大型独立队列中的表现。
他们招募了676名参与者:中心的训练队列(n = 346;43名PSP-P,194名PD,109名对照组)和一个国际研究小组的独立测试队列(n = 330;62名PSP-P,171名PD,97名对照组)。并开发了一种新的内部算法,用于MRPI 2.0的计算,并使用ROC曲线评估其在区分PSP-P和PD以及两个队列的对照受试者方面的表现。
他们发现:自动MRPI 2.0在区分PSP-P患者和PD患者以及对照组患者方面表现出色(ROC面积[AUC]=0.93[95%置信区间,0. 89-0.98]和AUC=0.97[0.93-1.00])和国际测试队列(PSP-P与PD相比,AUC=0.92[0.87-0.97];
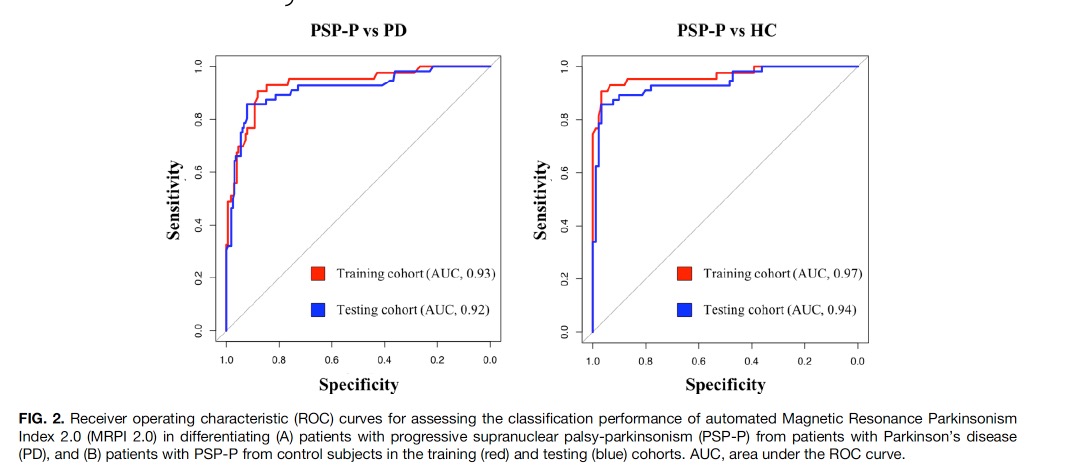 图2:论文结果图
图2:论文结果图
PSP-P与对照组相比,AUC=0.94[0.90-0.98]),表明结果具有普适性。自动MRPI 2.0也能准确区分PSP-P和PD的早期疾病(AUC = 0.91 [0.84-0.97])。自动和手动MRPI 2.0值之间有很强的相关性(r = 0.91,P < 0.001)。
该研究的重要意义在于提供了一个自动化的、经过验证的、可推广的磁共振生物标志物来区分PSP-P和PD。使用MRPI 2.0自动算法而不是人工测量,对不同中心的PSP-P患者的测量标准化很重要,对多中心研究和涉及不同地域患者的临床试验有积极影响。
原文出处:
Quattrone A, Bianco MG, Antonini A, et al. Development and Validation of Automated Magnetic Resonance Parkinsonism Index 2.0 to Distinguish Progressive Supranuclear Palsy‐Parkinsonism From Parkinson’s Disease. _Movement Disorders_. Published online April 11, 2022:mds.28992. doi:[10.1002/mds.28992](https://doi.org/10.1002/mds.28992)
本网站所有内容来源注明为“梅斯医学”或“MedSci原创”的文字、图片和音视频资料,版权均属于梅斯医学所有。非经授权,任何媒体、网站或个人不得转载,授权转载时须注明来源为“梅斯医学”。其它来源的文章系转载文章,或“梅斯号”自媒体发布的文章,仅系出于传递更多信息之目的,本站仅负责审核内容合规,其内容不代表本站立场,本站不负责内容的准确性和版权。如果存在侵权、或不希望被转载的媒体或个人可与我们联系,我们将立即进行删除处理。
在此留言


















#ERS#
47
#进行性#
46
#Dis#
37
#disorders#
41
#disorder#
40
#Disord#
29