-
 Primary Multi-Systemic Metastases in Osteosarcoma: Presentation, Treatment, and Survival of 83 Patients of the Cooperative Osteosarcoma Study Group
Primary Multi-Systemic Metastases in Osteosarcoma: Presentation, Treatment, and Survival of 83 Patients of the Cooperative Osteosarcoma Study Group -
 Addressing Genetic Tumor Heterogeneity, Post-Therapy Metastatic Spread, Cancer Repopulation, and Development of Acquired Tumor Cell Resistance
Addressing Genetic Tumor Heterogeneity, Post-Therapy Metastatic Spread, Cancer Repopulation, and Development of Acquired Tumor Cell Resistance -
 The Role of Macrophages in Sarcoma Tumor Microenvironment and Treatment
The Role of Macrophages in Sarcoma Tumor Microenvironment and Treatment -
 Synergistic Sensitization of High-Grade Serous Ovarian Cancer Cells Lacking Caspase-8 Expression to Chemotherapeutics Using Combinations of Small-Molecule BRD4 and CDK9 Inhibitors
Synergistic Sensitization of High-Grade Serous Ovarian Cancer Cells Lacking Caspase-8 Expression to Chemotherapeutics Using Combinations of Small-Molecule BRD4 and CDK9 Inhibitors
Journal Description
Cancers
Cancers
is a peer-reviewed, open access journal of oncology, published semimonthly online by MDPI. The Irish Association for Cancer Research (IACR), Spanish Association for Cancer Research (ASEICA), Biomedical Research Centre (CIBM), British Neuro-Oncology Society (BNOS) and Spanish Group for Cancer Immuno-Biotherapy (GÉTICA) are affiliated with Cancers and their members receive a discount on the article processing charges.
- Open Access— free for readers, with article processing charges (APC) paid by authors or their institutions.
- High Visibility: indexed within Scopus, SCIE (Web of Science), PubMed, PMC, Embase, CAPlus / SciFinder, and other databases.
- Journal Rank: JCR - Q2 (Oncology) / CiteScore - Q1 (Oncology)
- Rapid Publication: manuscripts are peer-reviewed and a first decision is provided to authors approximately 17.9 days after submission; acceptance to publication is undertaken in 2.8 days (median values for papers published in this journal in the second half of 2023).
- Recognition of Reviewers: reviewers who provide timely, thorough peer-review reports receive vouchers entitling them to a discount on the APC of their next publication in any MDPI journal, in appreciation of the work done.
- Sections: published in 18 topical sections.
- Companion journals for Cancers include: Radiation and Onco.
Impact Factor:
5.2 (2022);
5-Year Impact Factor:
5.6 (2022)
Latest Articles
Focused Ultrasound-Enhanced Liquid Biopsy: A Promising Diagnostic Tool for Brain Tumor Patients
Cancers 2024, 16(8), 1576; https://doi.org/10.3390/cancers16081576 (registering DOI) - 19 Apr 2024
Abstract
The performance of minimally invasive molecular diagnostic tools in brain tumors, such as liquid biopsy, has so far been limited by the blood–brain barrier (BBB). The BBB hinders the release of brain tumor biomarkers into the bloodstream. The use of focused ultrasound in
[...] Read more.
The performance of minimally invasive molecular diagnostic tools in brain tumors, such as liquid biopsy, has so far been limited by the blood–brain barrier (BBB). The BBB hinders the release of brain tumor biomarkers into the bloodstream. The use of focused ultrasound in conjunction with microbubbles has been shown to temporarily open the BBB (FUS-BBBO). This may enhance blood-based tumor biomarker levels. This systematic review provides an overview of the data regarding FUS-BBBO-enhanced liquid biopsy for primary brain tumors. A systematic search was conducted in PubMed and Embase databases with key terms “brain tumors”, “liquid biopsy”, “FUS” and their synonyms, in accordance with PRISMA statement guidelines. Five preclinical and two clinical studies were included. Preclinical studies utilized mouse, rat and porcine glioma models. Biomarker levels were found to be higher in sonicated groups compared to control groups. Both stable and inertial microbubble cavitation increased biomarker levels, whereas only inertial cavitation induced microhemorrhages. In clinical studies involving 14 patients with high-grade brain tumors, biomarker levels were increased after FUS-BBBO with stable cavitation. In conclusion, FUS-BBBO-enhanced liquid biopsy using stable cavitation shows diagnostic potential for primary brain tumors. Further research is imperative before integrating FUS-BBBO for liquid biopsy enhancement into clinical practice.
Full article
(This article belongs to the Special Issue New Strategies in Diagnosis and Treatments for Brain Tumors (Volume II))
Open AccessReview
The Role of Estrogen and Estrogen Receptors in Head and Neck Tumors
by
Jacqueline-Katrin Kranjčević, Josipa Čonkaš and Petar Ozretić
Cancers 2024, 16(8), 1575; https://doi.org/10.3390/cancers16081575 - 19 Apr 2024
Abstract
Head and neck squamous cell carcinoma (HNSCC) is the most common histological form of head and neck tumors (HNTs), which originate from the epithelium of the lips and oral cavity, pharynx, larynx, salivary glands, nasal cavity, and sinuses. The main risk factors include
[...] Read more.
Head and neck squamous cell carcinoma (HNSCC) is the most common histological form of head and neck tumors (HNTs), which originate from the epithelium of the lips and oral cavity, pharynx, larynx, salivary glands, nasal cavity, and sinuses. The main risk factors include consumption of tobacco in all forms and alcohol, as well as infections with high-risk human papillomaviruses or the Epstein–Barr virus. Regardless of the etiological agent, the risk of developing different types of HNTs is from two to more than six times higher in males than in females. The reason for such disparities probably lies in a combination of both biological and psychosocial factors. Therefore, it is hypothesized that exposure to female sex hormones, primarily estrogen, provides women with protection against the formation and metastasis of HNTs. In this review, we synthesized available knowledge on the role of estrogen and estrogen receptors (ERs) in the development and progression of HNTs, with special emphasis on membrane ERs, which are much less studied. We can summarize that in addition to epidemiologic studies unequivocally pointing to the protective effect of estrogen in women, an increased expression of both nuclear ERs, ERα, and ERβ, and membrane ERs, ERα36, GPER1, and NaV1.2, was present in different types of HNSCC, for which anti-estrogens could be used as an effective therapeutic approach.
Full article
(This article belongs to the Special Issue Estrogens and Estrogen Receptor Modulators in Cancer Research and Therapy (Volume II))
Open AccessArticle
The Impact of Lateral Ventricular Opening in the Resection of Newly Diagnosed High-Grade Gliomas: A Single Center Experience
by
Fabio Cofano, Andrea Bianconi, Raffaele De Marco, Elena Consoli, Pietro Zeppa, Francesco Bruno, Alessia Pellerino, Flavio Panico, Luca Francesco Salvati, Francesca Rizzo, Alberto Morello, Roberta Rudà, Giovanni Morana, Antonio Melcarne and Diego Garbossa
Cancers 2024, 16(8), 1574; https://doi.org/10.3390/cancers16081574 - 19 Apr 2024
Abstract
Given the importance of maximizing resection for prognosis in patients with HGG and the potential risks associated with ventricle opening, this study aimed to assess the actual increase in post-surgical complications related to lateral ventricle opening and its influence on OS and PFS.
[...] Read more.
Given the importance of maximizing resection for prognosis in patients with HGG and the potential risks associated with ventricle opening, this study aimed to assess the actual increase in post-surgical complications related to lateral ventricle opening and its influence on OS and PFS. A retrospective study was conducted on newly diagnosed HGG, dividing the patients into two groups according to whether the lateral ventricle was opened (69 patients) or not opened (311 patients). PFS, OS, subependymal dissemination, distant parenchymal recurrences, the development of hydrocephalus and CSF leak were considered outcome measures. A cohort of 380 patients (154 females (40.5%) and 226 males (59.5%)) was involved in the study (median age 61 years). The PFS averaged 10.9 months (±13.3 SD), and OS averaged 16.6 months (± 16.3 SD). Among complications, subependymal dissemination was registered in 15 cases (3.9%), multifocal and multicentric progression in 56 cases (14.7%), leptomeningeal dissemination in 12 (3.2%) and hydrocephalus in 8 (2.1%). These occurrences could not be clearly justified by ventricular opening. The act of opening the lateral ventricles itself does not carry an elevated risk of dissemination, hydrocephalus or cerebrospinal fluid (CSF) leak. Therefore, if necessary, it should be pursued to achieve radical removal of the disease.
Full article
(This article belongs to the Section Methods and Technologies Development)
Open AccessReview
DNA Damage Responses in Tumors Are Not Proliferative Stimuli, but Rather They Are DNA Repair Actions Requiring Supportive Medical Care
by
Zsuzsanna Suba
Cancers 2024, 16(8), 1573; https://doi.org/10.3390/cancers16081573 - 19 Apr 2024
Abstract
Background: In tumors, somatic mutagenesis presumably drives the DNA damage response (DDR) via altered regulatory pathways, increasing genomic instability and proliferative activity. These considerations led to the standard therapeutic strategy against cancer: the disruption of mutation-activated DNA repair pathways of tumors.Purpose: Justifying that
[...] Read more.
Background: In tumors, somatic mutagenesis presumably drives the DNA damage response (DDR) via altered regulatory pathways, increasing genomic instability and proliferative activity. These considerations led to the standard therapeutic strategy against cancer: the disruption of mutation-activated DNA repair pathways of tumors.Purpose: Justifying that cancer cells are not enemies to be killed, but rather that they are ill human cells which have the remnants of physiologic regulatory pathways. Results: 1. Genomic instability and cancer development may be originated from a flaw in estrogen signaling rather than excessive estrogen signaling; 2. Healthy cells with genomic instability exhibit somatic mutations, helping DNA restitution; 3. Somatic mutations in tumor cells aim for the restoration of DNA damage, rather than further genomic derangement; 4. In tumors, estrogen signaling drives the pathways of DNA stabilization, leading to apoptotic death; 5. In peritumoral cellular infiltration, the genomic damage of the tumor induces inflammatory cytokine secretion and increased estrogen synthesis. In the inflammatory cells, an increased growth factor receptor (GFR) signaling confers the unliganded activation of estrogen receptors (ERs); 6. In breast cancer cells responsive to genotoxic therapy, constitutive mutations help the upregulation of estrogen signaling and consequential apoptosis. In breast tumors non-responsive to genotoxic therapy, the possibilities for ER activation via either liganded or unliganded pathways are exhausted, leading to farther genomic instability and unrestrained proliferation. Conclusions: Understanding the real character and behavior of human tumors at the molecular level suggests that we should learn the genome repairing methods of tumors and follow them by supportive therapy, rather than provoking additional genomic damages.
Full article
(This article belongs to the Topic Recent Advances in Anticancer Strategies)
►▼
Show Figures
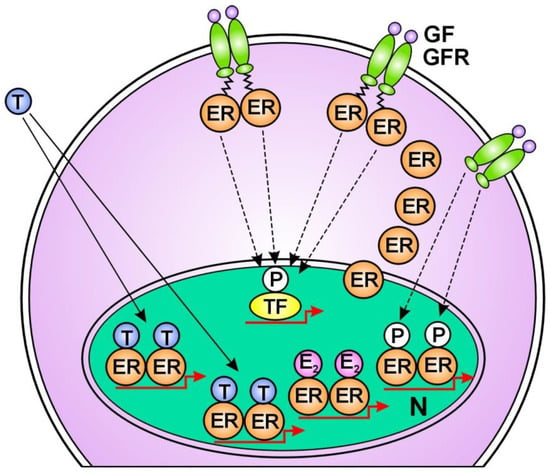
Figure 1
Open AccessArticle
The Genomic, Transcriptomic, and Immunologic Landscape of HRAS Mutations in Solid Tumors
by
Samuel A. Kareff, Asaad Trabolsi, Harris B. Krause, Timothy Samec, Andrew Elliott, Estelamari Rodriguez, Coral Olazagasti, Dionysios C. Watson, Matias A. Bustos, Dave S. B. Hoon, Stephanie L. Graff, Emmanuel S. Antonarakis, Sanjay Goel, George Sledge and Gilberto Lopes
Cancers 2024, 16(8), 1572; https://doi.org/10.3390/cancers16081572 - 19 Apr 2024
Abstract
Tipifarnib is the only targeted therapy breakthrough for HRAS-mutant (HRASmt) recurrent or metastatic head and neck squamous cell carcinoma (HNSCC). The molecular profiles of HRASmt cancers are difficult to explore given the low frequency of HRASmt. This study
[...] Read more.
Tipifarnib is the only targeted therapy breakthrough for HRAS-mutant (HRASmt) recurrent or metastatic head and neck squamous cell carcinoma (HNSCC). The molecular profiles of HRASmt cancers are difficult to explore given the low frequency of HRASmt. This study aims to understand the molecular co-alterations, immune profiles, and clinical outcomes of 524 HRASmt solid tumors including urothelial carcinoma (UC), breast cancer (BC), non-small-cell lung cancer (NSCLC), melanoma, and HNSCC. HRASmt was most common in UC (3.0%), followed by HNSCC (2.82%), melanoma (1.05%), BC (0.45%), and NSCLC (0.44%). HRASmt was absent in Her2+ BC regardless of hormone receptor status. HRASmt was more frequently associated with squamous compared to non-squamous NSCLC (60% vs. 40% in HRASwt, p = 0.002). The tumor microenvironment (TME) of HRASmt demonstrated increased M1 macrophages in triple-negative BC (TNBC), HNSCC, squamous NSCLC, and UC; increased M2 macrophages in TNBC; and increased CD8+ T-cells in HNSCC (all p < 0.05). Finally, HRASmt was associated with shorter overall survival in HNSCC (HR: 1.564, CI: 1.16–2.11, p = 0.003) but not in the other cancer types examined. In conclusion, this study provides new insights into the unique molecular profiles of HRASmt tumors that may help to identify new targets and guide future clinical trial design.
Full article
(This article belongs to the Special Issue New Findings in Targeting Cancer Proteins)
►▼
Show Figures
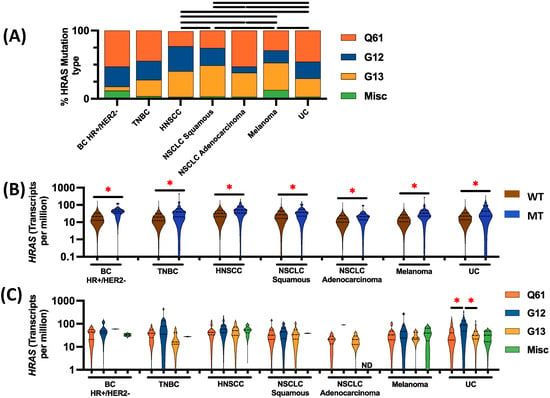
Figure 1
Open AccessReview
Current State of Melanoma Therapy and Next Steps: Battling Therapeutic Resistance
by
Anna Fateeva, Kevinn Eddy and Suzie Chen
Cancers 2024, 16(8), 1571; https://doi.org/10.3390/cancers16081571 - 19 Apr 2024
Abstract
Melanoma is the most aggressive and deadly form of skin cancer due to its high propensity to metastasize to distant organs. Significant progress has been made in the last few decades in melanoma therapeutics, most notably in targeted therapy and immunotherapy. These approaches
[...] Read more.
Melanoma is the most aggressive and deadly form of skin cancer due to its high propensity to metastasize to distant organs. Significant progress has been made in the last few decades in melanoma therapeutics, most notably in targeted therapy and immunotherapy. These approaches have greatly improved treatment response outcomes; however, they remain limited in their abilities to hinder disease progression due, in part, to the onset of acquired resistance. In parallel, intrinsic resistance to therapy remains an issue to be resolved. In this review, we summarize currently available therapeutic options for melanoma treatment and focus on possible mechanisms that drive therapeutic resistance. A better understanding of therapy resistance will provide improved rational strategies to overcome these obstacles.
Full article
(This article belongs to the Section Cancer Therapy)
Open AccessArticle
Machine Learning Applied to Pre-Operative Computed-Tomography-Based Radiomic Features Can Accurately Differentiate Uterine Leiomyoma from Leiomyosarcoma: A Pilot Study
by
Miriam Santoro, Vladislav Zybin, Camelia Alexandra Coada, Giulia Mantovani, Giulia Paolani, Marco Di Stanislao, Cecilia Modolon, Stella Di Costanzo, Andrei Lebovici, Gloria Ravegnini, Antonio De Leo, Marco Tesei, Pietro Pasquini, Luigi Lovato, Alessio Giuseppe Morganti, Maria Abbondanza Pantaleo, Pierandrea De Iaco, Lidia Strigari and Anna Myriam Perrone
Cancers 2024, 16(8), 1570; https://doi.org/10.3390/cancers16081570 - 19 Apr 2024
Abstract
Background: The accurate discrimination of uterine leiomyosarcomas and leiomyomas in a pre-operative setting remains a current challenge. To date, the diagnosis is made by a pathologist on the excised tumor. The aim of this study was to develop a machine learning algorithm using
[...] Read more.
Background: The accurate discrimination of uterine leiomyosarcomas and leiomyomas in a pre-operative setting remains a current challenge. To date, the diagnosis is made by a pathologist on the excised tumor. The aim of this study was to develop a machine learning algorithm using radiomic data extracted from contrast-enhanced computed tomography (CECT) images that could accurately distinguish leiomyosarcomas from leiomyomas. Methods: Pre-operative CECT images from patients submitted to surgery with a histological diagnosis of leiomyoma or leiomyosarcoma were used for the region of interest identification and radiomic feature extraction. Feature extraction was conducted using the PyRadiomics library, and three feature selection methods combined with the general linear model (GLM), random forest (RF), and support vector machine (SVM) classifiers were built, trained, and tested for the binary classification task (malignant vs. benign). In parallel, radiologists assessed the diagnosis with or without clinical data. Results: A total of 30 patients with leiomyosarcoma (mean age 59 years) and 35 patients with leiomyoma (mean age 48 years) were included in the study, comprising 30 and 51 lesions, respectively. Out of nine machine learning models, the three feature selection methods combined with the GLM and RF classifiers showed good performances, with predicted area under the curve (AUC), sensitivity, and specificity ranging from 0.78 to 0.97, from 0.78 to 1.00, and from 0.67 to 0.93, respectively, when compared to the results obtained from experienced radiologists when blinded to the clinical profile (AUC = 0.73 95%CI = 0.62–0.84), as well as when the clinical data were consulted (AUC = 0.75 95%CI = 0.65–0.85). Conclusions: CECT images integrated with radiomics have great potential in differentiating uterine leiomyomas from leiomyosarcomas. Such a tool can be used to mitigate the risks of eventual surgical spread in the case of leiomyosarcoma and allow for safer fertility-sparing treatment in patients with benign uterine lesions.
Full article
(This article belongs to the Special Issue Innovations in Diagnosis, Prognostic Evaluation, and Therapeutic Management of Gynecologic Tumors)
►▼
Show Figures
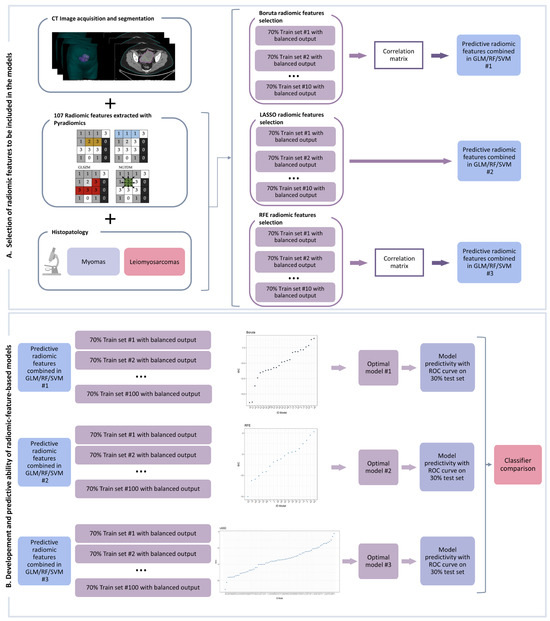
Figure 1
Open AccessReview
CD44: A New Prognostic Marker in Colorectal Cancer?
by
Pina Ziranu, Andrea Pretta, Valentina Aimola, Flaviana Cau, Stefano Mariani, Alessandra Pia D’Agata, Claudia Codipietro, Daiana Rizzo, Veronica Dell’Utri, Giorgia Sanna, Giusy Moledda, Andrea Cadoni, Eleonora Lai, Marco Puzzoni, Valeria Pusceddu, Massimo Castagnola, Mario Scartozzi and Gavino Faa
Cancers 2024, 16(8), 1569; https://doi.org/10.3390/cancers16081569 - 19 Apr 2024
Abstract
Cluster of differentiation 44 (CD44) is a non-kinase cell surface glycoprotein. It is overexpressed in several cell types, including cancer stem cells (CSCs). Cells overexpressing CD44 exhibit several CSC traits, such as self-renewal, epithelial–mesenchymal transition (EMT) capability, and resistance to chemo- and radiotherapy.
[...] Read more.
Cluster of differentiation 44 (CD44) is a non-kinase cell surface glycoprotein. It is overexpressed in several cell types, including cancer stem cells (CSCs). Cells overexpressing CD44 exhibit several CSC traits, such as self-renewal, epithelial–mesenchymal transition (EMT) capability, and resistance to chemo- and radiotherapy. The role of CD44 in maintaining stemness and the CSC function in tumor progression is accomplished by binding to its main ligand, hyaluronan (HA). The HA-CD44 complex activates several signaling pathways that lead to cell proliferation, adhesion, migration, and invasion. The CD44 gene regularly undergoes alternative splicing, resulting in the standard (CD44s) and variant (CD44v) isoforms. The different functional roles of CD44s and specific CD44v isoforms still need to be fully understood. The clinicopathological impact of CD44 and its isoforms in promoting tumorigenesis suggests that CD44 could be a molecular target for cancer therapy. Furthermore, the recent association observed between CD44 and KRAS-dependent carcinomas and the potential correlations between CD44 and tumor mutational burden (TMB) and microsatellite instability (MSI) open new research scenarios for developing new strategies in cancer treatment. This review summarises current research regarding the different CD44 isoform structures, their roles, and functions in supporting tumorigenesis and discusses its therapeutic implications.
Full article
(This article belongs to the Special Issue The Biology of CD44 and Its Role in Cancer Progression: Therapeutic Implications)
Open AccessReview
Coagulation Protease-Driven Cancer Immune Evasion: Potential Targets for Cancer Immunotherapy
by
Subhojit Paul, Tanmoy Mukherjee and Kaushik Das
Cancers 2024, 16(8), 1568; https://doi.org/10.3390/cancers16081568 - 19 Apr 2024
Abstract
Blood coagulation and cancer are intrinsically connected, hypercoagulation-associated thrombotic complications are commonly observed in certain types of cancer, often leading to decreased survival in cancer patients. Apart from the common role in coagulation, coagulation proteases often trigger intracellular signaling in various cancers via
[...] Read more.
Blood coagulation and cancer are intrinsically connected, hypercoagulation-associated thrombotic complications are commonly observed in certain types of cancer, often leading to decreased survival in cancer patients. Apart from the common role in coagulation, coagulation proteases often trigger intracellular signaling in various cancers via the activation of a G protein-coupled receptor superfamily protease: protease-activated receptors (PARs). Although the role of PARs is well-established in the development and progression of certain types of cancer, their impact on cancer immune response is only just emerging. The present review highlights how coagulation protease-driven PAR signaling plays a key role in modulating innate and adaptive immune responses. This is followed by a detailed discussion on the contribution of coagulation protease-induced signaling in cancer immune evasion, thereby supporting the growth and development of certain tumors. A special section of the review demonstrates the role of coagulation proteases, thrombin, factor VIIa, and factor Xa in cancer immune evasion. Targeting coagulation protease-induced signaling might be a potential therapeutic strategy to boost the immune surveillance mechanism of a host fighting against cancer, thereby augmenting the clinical consequences of targeted immunotherapeutic regimens.
Full article
(This article belongs to the Special Issue Existing and Emerging Biomarkers for Immune Checkpoint Immunotherapy in Solid Tumors)
►▼
Show Figures
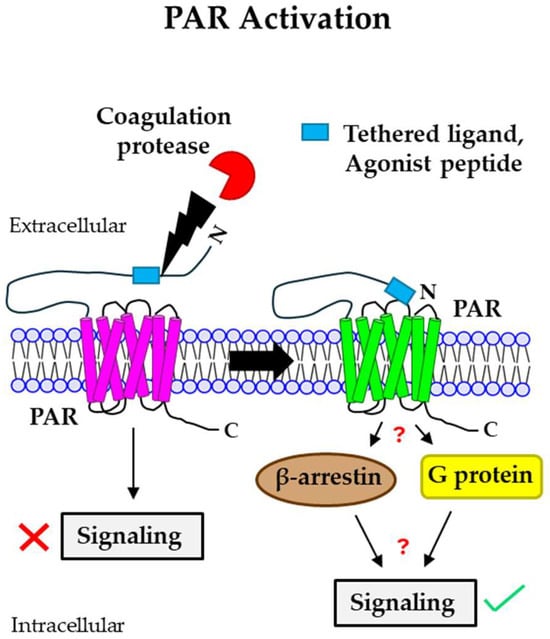
Figure 1
Open AccessArticle
Discovery of Novel Potential Prognostic Markers and Targeted Therapy to Overcome Chemotherapy Resistance in an Advanced-Stage Wilms Tumor
by
Pongsakorn Choochuen, Natakorn Nokchan, Natthapon Khongcharoen, Wison Laochareonsuk, Komwit Surachat, Thirachit Chotsampancharoen, Thanit Sila and Surasak Sangkhathat
Cancers 2024, 16(8), 1567; https://doi.org/10.3390/cancers16081567 - 19 Apr 2024
Abstract
Wilms tumor (WT), the most prevalent type of renal cancer in children, exhibits overall survival rates exceeding 90%. However, chemotherapy resistance, which occurs in approximately 10% of WT cases, is a major challenge for the treatment of WT, particularly for advanced-stage patients. In
[...] Read more.
Wilms tumor (WT), the most prevalent type of renal cancer in children, exhibits overall survival rates exceeding 90%. However, chemotherapy resistance, which occurs in approximately 10% of WT cases, is a major challenge for the treatment of WT, particularly for advanced-stage patients. In this study, we aimed to discover potential mutation markers and drug targets associated with chemotherapy resistance in advanced-stage WT. We performed exome sequencing to detect somatic mutations and molecular targets in 43 WT samples, comprising 26 advanced-stage WTs, of which 7 cases were chemotherapy-resistant. Our analysis revealed four genes (ALPK2, C16orf96, PRKDC, and SVIL) that correlated with chemotherapy resistance and reduced disease-free survival in advanced-stage WT. Additionally, we identified driver mutations in 55 genes within the chemotherapy-resistant group, including 14 druggable cancer driver genes. Based on the mutation profiles of the resistant WT samples, we propose potential therapeutic strategies involving platinum-based agents, PARP inhibitors, and antibiotic/antineoplastic agents. Our findings provide insights into the genetic landscape of WT and offer potential avenues for targeted treatment, particularly for patients with chemotherapy resistance.
Full article
(This article belongs to the Section Cancer Biomarkers)
►▼
Show Figures
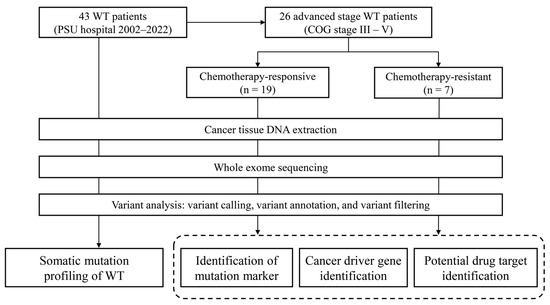
Figure 1
Open AccessReview
Advancements in Image-Based Models for High-Grade Gliomas Might Be Accelerated
by
Guido Frosina
Cancers 2024, 16(8), 1566; https://doi.org/10.3390/cancers16081566 - 19 Apr 2024
Abstract
The first half of 2022 saw the publication of several major research advances in image-based models and artificial intelligence applications to optimize treatment strategies for high-grade gliomas, the deadliest brain tumors. We review them and discuss the barriers that delay their entry into
[...] Read more.
The first half of 2022 saw the publication of several major research advances in image-based models and artificial intelligence applications to optimize treatment strategies for high-grade gliomas, the deadliest brain tumors. We review them and discuss the barriers that delay their entry into clinical practice; particularly, the small sample size and the heterogeneity of the study designs and methodologies used. We will also write about the poor and late palliation that patients suffering from high-grade glioma can count on at the end of life, as well as the current legislative instruments, with particular reference to Italy. We suggest measures to accelerate the gradual progress in image-based models and end of life care for patients with high-grade glioma.
Full article
(This article belongs to the Special Issue Radiobiological Modelling in the New Era of Precision Radiation Oncology)
Open AccessArticle
Genetic Diagnosis of Retinoblastoma Using Aqueous Humour—Findings from an Extended Cohort
by
Amy Gerrish, Chipo Mashayamombe-Wolfgarten, Edward Stone, Claudia Román-Montañana, Joseph Abbott, Helen Jenkinson, Gerard Millen, Sam Gurney, Maureen McCalla, Sarah-Jane Staveley, Anu Kainth, Maria Kirk, Claire Bowen, Susan Cavanagh, Sancha Bunstone, Megan Carney, Ajay Mohite, Samuel Clokie, M. Ashwin Reddy, Alison Foster, Stephanie Allen, Manoj Parulekar and Trevor Coleadd
Show full author list
remove
Hide full author list
Cancers 2024, 16(8), 1565; https://doi.org/10.3390/cancers16081565 (registering DOI) - 19 Apr 2024
Abstract
The identification of somatic RB1 variation is crucial to confirm the heritability of retinoblastoma. We and others have previously shown that, when tumour DNA is unavailable, cell-free DNA (cfDNA) derived from aqueous humour (AH) can be used to identify somatic RB1 pathogenic variation.
[...] Read more.
The identification of somatic RB1 variation is crucial to confirm the heritability of retinoblastoma. We and others have previously shown that, when tumour DNA is unavailable, cell-free DNA (cfDNA) derived from aqueous humour (AH) can be used to identify somatic RB1 pathogenic variation. Here we report RB1 pathogenic variant detection, as well as cfDNA concentration in an extended cohort of 75 AH samples from 68 patients. We show cfDNA concentration is highly variable and significantly correlated with the collection point of the AH. Cell-free DNA concentrations above 5 pg/µL enabled the detection of 93% of known or expected RB1 pathogenic variants. In AH samples collected during intravitreal chemotherapy treatment (Tx), the yield of cfDNA above 5 pg/µL and subsequent variant detection was low (≤46%). However, AH collected by an anterior chamber tap after one to three cycles of primary chemotherapy (Dx1+) enabled the detection of 75% of expected pathogenic variants. Further limiting our analysis to Dx1+ samples taken after ≤2 cycles (Dx ≤ 2) provided measurable levels of cfDNA in all cases, and a subsequent variant detection rate of 95%. Early AH sampling is therefore likely to be important in maximising cfDNA concentration and the subsequent detection of somatic RB1 pathogenic variants in retinoblastoma patients undergoing conservative treatment.
Full article
(This article belongs to the Section Cancer Causes, Screening and Diagnosis)
Open AccessArticle
Enhancements in Radiological Detection of Metastatic Lymph Nodes Utilizing AI-Assisted Ultrasound Imaging Data and the Lymph Node Reporting and Data System Scale
by
Cezary Chudobiński, Bartosz Świderski, Izabella Antoniuk and Jarosław Kurek
Cancers 2024, 16(8), 1564; https://doi.org/10.3390/cancers16081564 - 19 Apr 2024
Abstract
The paper presents a novel approach for the automatic detection of neoplastic lesions in lymph nodes (LNs). It leverages the latest advances in machine learning (ML) with the LN Reporting and Data System (LN-RADS) scale. By integrating diverse datasets and network structures, the
[...] Read more.
The paper presents a novel approach for the automatic detection of neoplastic lesions in lymph nodes (LNs). It leverages the latest advances in machine learning (ML) with the LN Reporting and Data System (LN-RADS) scale. By integrating diverse datasets and network structures, the research investigates the effectiveness of ML algorithms in improving diagnostic accuracy and automation potential. Both Multinominal Logistic Regression (MLR)-integrated and fully connected neuron layers are included in the analysis. The methods were trained using three variants of combinations of histopathological data and LN-RADS scale labels to assess their utility. The findings demonstrate that the LN-RADS scale improves prediction accuracy. MLR integration is shown to achieve higher accuracy, while the fully connected neuron approach excels in AUC performance. All of the above suggests a possibility for significant improvement in the early detection and prognosis of cancer using AI techniques. The study underlines the importance of further exploration into combined datasets and network architectures, which could potentially lead to even greater improvements in the diagnostic process.
Full article
(This article belongs to the Section Cancer Metastasis)
Open AccessReview
Latest Insights and Therapeutic Advances in Myelodysplastic Neoplasms
by
Pasquale Niscola, Valentina Gianfelici, Marco Giovannini, Daniela Piccioni, Carla Mazzone and Paolo de Fabritiis
Cancers 2024, 16(8), 1563; https://doi.org/10.3390/cancers16081563 - 19 Apr 2024
Abstract
Myelodysplastic syndromes/neoplasms (MDSs) encompass a range of hematopoietic malignancies, commonly affecting elderly individuals. Molecular alterations in the hematopoietic stem cell compartment drive disease pathogenesis. Recent advancements in genomic profiling have provided valuable insights into the biological underpinnings of MDSs and have expanded therapeutic
[...] Read more.
Myelodysplastic syndromes/neoplasms (MDSs) encompass a range of hematopoietic malignancies, commonly affecting elderly individuals. Molecular alterations in the hematopoietic stem cell compartment drive disease pathogenesis. Recent advancements in genomic profiling have provided valuable insights into the biological underpinnings of MDSs and have expanded therapeutic options, particularly for specific molecularly defined subgroups. This review highlights the diagnostic principles, classification updates, prognostic stratification systems, and novel treatments, which could inform future clinical trials and enhance the management of adult MDS patients, particularly for specific molecularly defined subgroups.
Full article
(This article belongs to the Section Cancer Therapy)
►▼
Show Figures
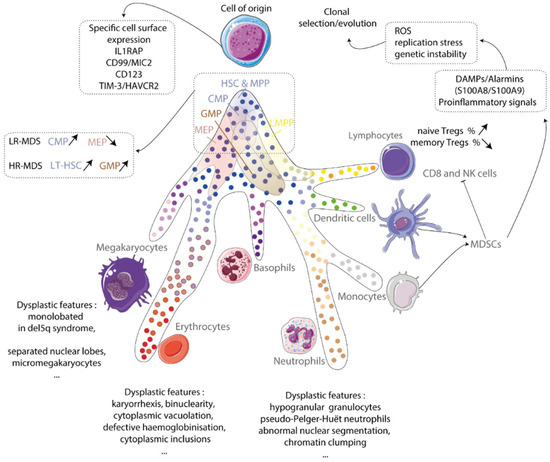
Figure 1
Open AccessArticle
Safety and Outcomes of Inferior Vena Cava Filter Placement in Oncology Patients: A Single-Centre Experience
by
Paweł Kurzyna, Marta Banaszkiewicz, Michał Florczyk, Jarosław Kępski, Michał Piłka, Piotr Kędzierski, Rafał Mańczak, Piotr Szwed, Krzysztof Kasperowicz, Katarzyna Wrona, Grzegorz Doroszewski, Adam Torbicki, Marcin Kurzyna, Sebastian Szmit and Szymon Darocha
Cancers 2024, 16(8), 1562; https://doi.org/10.3390/cancers16081562 - 19 Apr 2024
Abstract
The risk of venous thromboembolism (VTE) in the oncology population is significantly higher than in non-cancer patients. Inferior vena cava (IVC) filters may, therefore, be an important part of VTE treatment. In this study, we address the outcomes of placing IVC filters in
[...] Read more.
The risk of venous thromboembolism (VTE) in the oncology population is significantly higher than in non-cancer patients. Inferior vena cava (IVC) filters may, therefore, be an important part of VTE treatment. In this study, we address the outcomes of placing IVC filters in the oncology population. This single-centre, observational, retrospective study included 62 patients with active malignancy and acute VTE who underwent an IVC filter implantation due to contraindications to anticoagulation during the period 2012–2023. The control group consisted of 117 trauma patients. In both groups, an urgent surgical procedure requiring temporary cessation of anticoagulation was the most noted reason for IVC filter placement—76% in the oncology group vs. 100% in the non-oncology group (p < 0.001). No complications were reported during the IVC filter implantation procedures. There was no recurrence of pulmonary embolism or deep venous thrombosis in the oncology group after filter implantation. The rate of successful filter explantation, median time to retrieval, and abnormal findings during retrieval were not significantly different between both subgroups (64.3% vs. 76.5%, p = 0.334; 77 days vs. 84 days, p = 0.764; 61.5% vs. 54.2%, p = 0.672; respectively). The study showed that IVC filter placement is a safe and effective method of preventing PE in cancer patients with contraindications to anticoagulation. The complication rate following IVC filter implantation in cancer patients is low and similar to that in non-oncology patients.
Full article
(This article belongs to the Section Cancer Survivorship and Quality of Life)
►▼
Show Figures
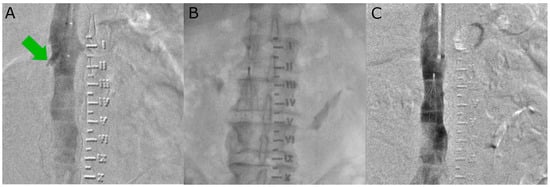
Figure 1
Open AccessArticle
NGS-Guided Precision Oncology in Breast Cancer and Gynecological Tumors—A Retrospective Molecular Tumor Board Analysis
by
Niklas Gremke, Fiona R. Rodepeter, Julia Teply-Szymanski, Sebastian Griewing, Jelena Boekhoff, Alina Stroh, Thomas S. Tarawneh, Jorge Riera-Knorrenschild, Christina Balser, Akira Hattesohl, Martin Middeke, Petra Ross, Anne-Sophie Litmeyer, Marcel Romey, Thorsten Stiewe, Thomas Wündisch, Andreas Neubauer, Carsten Denkert, Uwe Wagner and Elisabeth K. M. Mack
Cancers 2024, 16(8), 1561; https://doi.org/10.3390/cancers16081561 - 19 Apr 2024
Abstract
Background: Precision oncology treatments are being applied more commonly in breast and gynecological oncology through the implementation of Molecular Tumor Boards (MTBs), but real-world clinical outcome data remain limited. Methods: A retrospective analysis was conducted in patients with breast cancer (BC) and gynecological
[...] Read more.
Background: Precision oncology treatments are being applied more commonly in breast and gynecological oncology through the implementation of Molecular Tumor Boards (MTBs), but real-world clinical outcome data remain limited. Methods: A retrospective analysis was conducted in patients with breast cancer (BC) and gynecological malignancies referred to our center’s MTB from 2018 to 2023. The analysis covered patient characteristics, next-generation sequencing (NGS) results, MTB recommendations, therapy received, and clinical outcomes. Results: Sixty-three patients (77.8%) had metastatic disease, and forty-four patients (54.3%) had previously undergone three or more lines of systemic treatment. Personalized treatment recommendations were provided to 50 patients (63.3%), while 29 (36.7%) had no actionable target. Ultimately, 23 patients (29.1%) underwent molecular-matched treatment (MMT). Commonly altered genes in patients with pan-gyn tumors (BC and gynecological malignancies) included TP53 (n = 42/81, 51.9%), PIK3CA (n = 18/81, 22.2%), BRCA1/2 (n = 10/81, 12.3%), and ARID1A (n = 9/81, 11.1%). Patients treated with MMT showed significantly prolonged progression-free survival (median PFS 5.5 vs. 3.5 months, p = 0.0014). Of all patients who underwent molecular profiling, 13.6% experienced a major clinical benefit (PFSr ≥ 1.3 and PR/SD ≥ 6 months) through precision oncology. Conclusions: NGS-guided precision oncology demonstrated improved clinical outcomes in a subgroup of patients with gynecological and breast cancers.
Full article
(This article belongs to the Special Issue Genetics and Epigenetics of Gynecological Cancer)
►▼
Show Figures
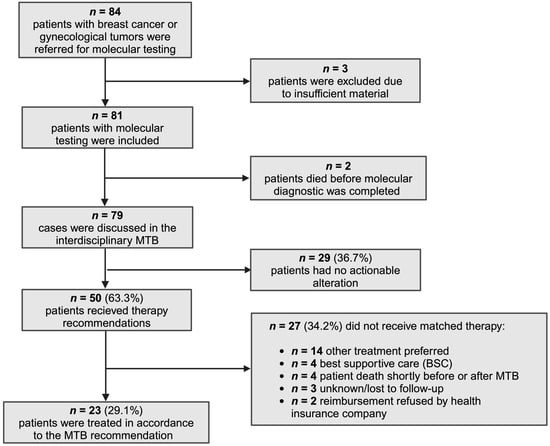
Figure 1
Open AccessReview
A Perspective Review: Analyzing Collagen Alterations in Ovarian Cancer by High-Resolution Optical Microscopy
by
Kristal L. Gant, Manish S. Patankar and Paul J. Campagnola
Cancers 2024, 16(8), 1560; https://doi.org/10.3390/cancers16081560 - 19 Apr 2024
Abstract
High-grade serous ovarian cancer (HGSOC) is the predominant subtype of ovarian cancer (OC), occurring in more than 80% of patients diagnosed with this malignancy. Histological and genetic analysis have confirmed the secretory epithelial of the fallopian tube (FT) as a major site of
[...] Read more.
High-grade serous ovarian cancer (HGSOC) is the predominant subtype of ovarian cancer (OC), occurring in more than 80% of patients diagnosed with this malignancy. Histological and genetic analysis have confirmed the secretory epithelial of the fallopian tube (FT) as a major site of origin of HGSOC. Although there have been significant strides in our understanding of this disease, early stage detection and diagnosis are still rare. Current clinical imaging modalities lack the ability to detect early stage pathogenesis in the fallopian tubes and the ovaries. However, there are several microscopic imaging techniques used to analyze the structural modifications in the extracellular matrix (ECM) protein collagen in ex vivo FT and ovarian tissues that potentially can be modified to fit the clinical setting. In this perspective, we evaluate and compare the myriad of optical tools available to visualize these alterations and the invaluable insights these data provide on HGSOC initiation. We also discuss the clinical implications of these findings and how these data may help novel tools for early diagnosis of HGSOC.
Full article
(This article belongs to the Special Issue Advances in Oncological Imaging)
►▼
Show Figures
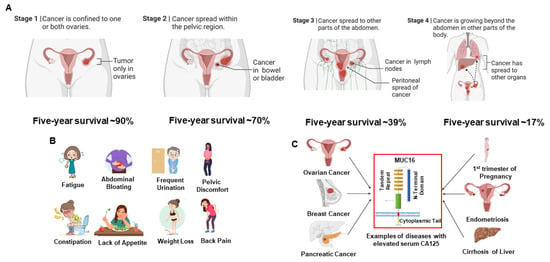
Figure 1
Open AccessArticle
Pressurised Intraperitoneal Aerosolised Chemotherapy—Results from the First Hundred Consecutive Procedures
by
David Hoskovec, Zdeněk Krška, Michal Vočka, Soňa Argalácsová and Petr Dytrych
Cancers 2024, 16(8), 1559; https://doi.org/10.3390/cancers16081559 - 19 Apr 2024
Abstract
PIPAC is a new and promising technique for the intraperitoneal administration of chemotherapy. It can be used in patients with various peritoneal cancer metastases. It is mainly a palliative treatment, but there is some neoadjuvant treatment potential. We have operated on 41 patients
[...] Read more.
PIPAC is a new and promising technique for the intraperitoneal administration of chemotherapy. It can be used in patients with various peritoneal cancer metastases. It is mainly a palliative treatment, but there is some neoadjuvant treatment potential. We have operated on 41 patients with various intra-abdominal cancers. PIPAC was performed every 6 weeks. The indication was extension of peritoneal carcinomatosis beyond the criteria for cytoreductive surgery and HIPEC. The effect was evaluated according to the peritoneal cancer index, the peritoneal regression grading score and the amount of ascites. Complications were classified according to the Clavien-Dindo system. We have performed 100 PIPAC procedures. There were two major complications, classified as Clavien Dindo III (2%). The number of procedures varied from 1 to 6. Five patients switched to cytoreductive surgery and HIPEC, and one was indicated for the watch and wait strategy due to total regression according to PRGS. Three patients are still continuing treatment. The others stopped treatment mainly because of progression of the disease and loss of metastases. We observed a reduction in ascites production soon after PIPAC application. PIPAC is a safe and well-tolerated treatment modality. It is mainly a palliative treatment that can improve the quality of life by reducing the production of ascites, but in about 10% of cases, it can reduce the extent of the disease and allow for further radical treatment.
Full article
(This article belongs to the Section Cancer Therapy)
►▼
Show Figures
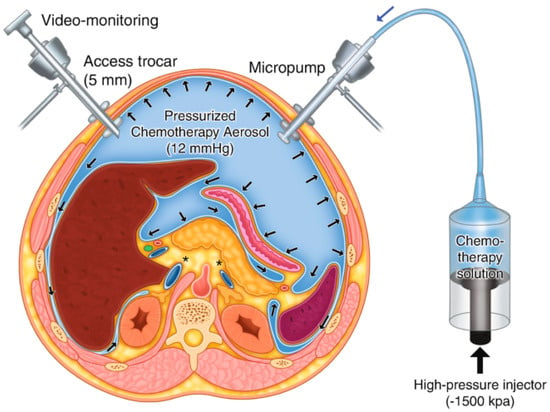
Figure 1
Open AccessReview
Therapeutic Strategies for RB1-Deficient Cancers: Intersecting Gene Regulation and Targeted Therapy
by
Mo-Fan Huang, Yuan-Xin Wang, Yu-Ting Chou and Dung-Fang Lee
Cancers 2024, 16(8), 1558; https://doi.org/10.3390/cancers16081558 - 19 Apr 2024
Abstract
The retinoblastoma (RB) transcriptional corepressor 1 (RB1) is a critical tumor suppressor gene, governing diverse cellular processes implicated in cancer biology. Dysregulation or deletion in RB1 contributes to the development and progression of various cancers, making it a prime target for therapeutic intervention.
[...] Read more.
The retinoblastoma (RB) transcriptional corepressor 1 (RB1) is a critical tumor suppressor gene, governing diverse cellular processes implicated in cancer biology. Dysregulation or deletion in RB1 contributes to the development and progression of various cancers, making it a prime target for therapeutic intervention. RB1′s canonical function in cell cycle control and DNA repair mechanisms underscores its significance in restraining aberrant cell growth and maintaining genomic stability. Understanding the complex interplay between RB1 and cellular pathways is beneficial to fully elucidate its tumor-suppressive role across different cancer types and for therapeutic development. As a result, investigating vulnerabilities arising from RB1 deletion-associated mechanisms offers promising avenues for targeted therapy. Recently, several findings highlighted multiple methods as a promising strategy for combating tumor growth driven by RB1 loss, offering potential clinical benefits in various cancer types. This review summarizes the multifaceted role of RB1 in cancer biology and its implications for targeted therapy.
Full article
(This article belongs to the Special Issue Genes in Cancer)
►▼
Show Figures
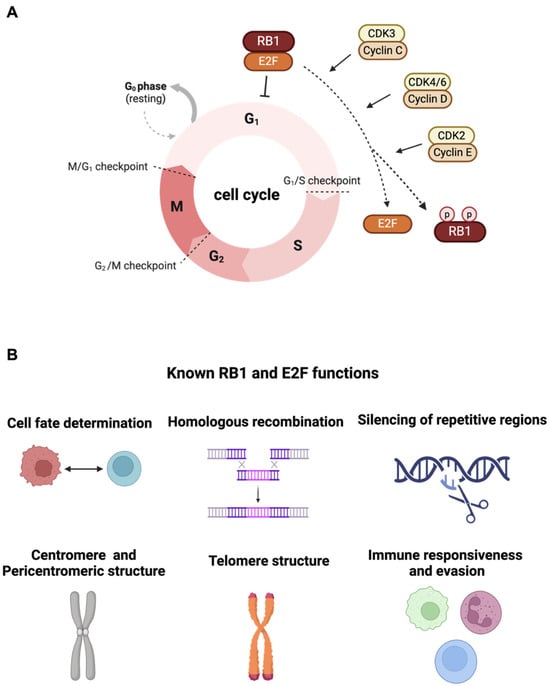
Figure 1
Open AccessReview
Glioma Stem Cells—Features for New Therapy Design
by
Nives Pećina-Šlaus and Reno Hrašćan
Cancers 2024, 16(8), 1557; https://doi.org/10.3390/cancers16081557 - 19 Apr 2024
Abstract
On a molecular level, glioma is very diverse and presents a whole spectrum of specific genetic and epigenetic alterations. The tumors are unfortunately resistant to available therapies and the survival rate is low. The explanation of significant intra- and inter-tumor heterogeneity and the
[...] Read more.
On a molecular level, glioma is very diverse and presents a whole spectrum of specific genetic and epigenetic alterations. The tumors are unfortunately resistant to available therapies and the survival rate is low. The explanation of significant intra- and inter-tumor heterogeneity and the infiltrative capability of gliomas, as well as its resistance to therapy, recurrence and aggressive behavior, lies in a small subset of tumor-initiating cells that behave like stem cells and are known as glioma cancer stem cells (GCSCs). They are responsible for tumor plasticity and are influenced by genetic drivers. Additionally, GCSCs also display greater migratory abilities. A great effort is under way in order to find ways to eliminate or neutralize GCSCs. Many different treatment strategies are currently being explored, including modulation of the tumor microenvironment, posttranscriptional regulation, epigenetic modulation and immunotherapy.
Full article
(This article belongs to the Special Issue Recent Advances in Rare Cancers: From Bench to Bedside and Back)
►▼
Show Figures
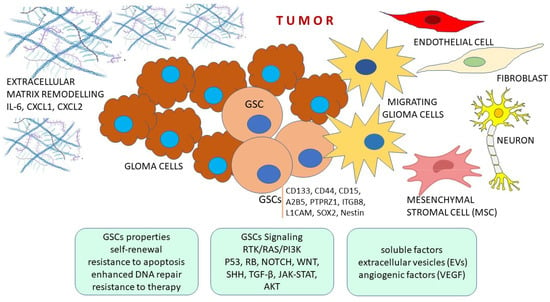
Figure 1

Journal Menu
► ▼ Journal Menu-
- Cancers Home
- Aims & Scope
- Editorial Board
- Reviewer Board
- Topical Advisory Panel
- Instructions for Authors
- Special Issues
- Topics
- Sections & Collections
- Article Processing Charge
- Indexing & Archiving
- Editor’s Choice Articles
- Most Cited & Viewed
- Journal Statistics
- Journal History
- Journal Awards
- Society Collaborations
- Conferences
- Editorial Office
Journal Browser
► ▼ Journal BrowserHighly Accessed Articles
Latest Books
E-Mail Alert
News
Topics
Topic in
Biomedicines, BioMedInformatics, Cancers, JCM, Cells, Current Oncology
Cancer Immunity and Immunotherapy: Early Detection, Diagnosis, Systemic Treatments, Novel Biomarkers, and Resistance Mechanisms
Topic Editors: Tao Jiang, Yongchang ZhangDeadline: 20 April 2024
Topic in
Bioengineering, Biomolecules, Cancers, Diseases, Nanomaterials, Pharmaceutics
Dynamic Nano-Biomaterials in Tissue Regeneration and Cancer Therapies
Topic Editors: Ramar Thangam, Heemin Kang, Bibin G. Anand, Ramachandran Vijayan, Venugopal KrishnanDeadline: 15 May 2024
Topic in
Biomedicines, Cancers, JFB, Nanomaterials, Polymers
Advanced Functional Materials for Regenerative Medicine
Topic Editors: Antonino Morabito, Luca ValentiniDeadline: 6 June 2024
Topic in
Biology, Cancers, Current Oncology, Diseases, JCM, Pathogens
Pathogenetic, Diagnostic and Therapeutic Perspectives in Head and Neck Cancer
Topic Editors: Shun-Fa Yang, Ming-Hsien ChienDeadline: 20 June 2024

Conferences
Special Issues
Special Issue in
Cancers
The Role of Tunneling Nanotubes in Intercellular Communication and Pathophysiology of Cancer
Guest Editor: Emil LouDeadline: 25 April 2024
Special Issue in
Cancers
Innovations in Diagnosis and Treatment of Colon and Rectal Cancer: Preoperative Optimisation, Multidisciplinary Management, and Surgical Technology Advancement
Guest Editor: Gianluca PellinoDeadline: 30 April 2024
Special Issue in
Cancers
Molecular and Cellular Heterogeneity in an Evolving Tumor Landscape: When Diversity Gives Rise to Aggressive and Drug Resistant Cells
Guest Editor: Michelle R. DawsonDeadline: 20 May 2024
Special Issue in
Cancers
Innovations in Soft Tissue Sarcoma Diagnosis and Treatment
Guest Editors: Erlinda M. Gordon, Sant P. Chawla, Frederick L. HallDeadline: 30 May 2024
Topical Collections
Topical Collection in
Cancers
Drug Resistance and Novel Therapies in Cancers
Collection Editor: Zhixiang Wang










