-
 Methylene Blue Metabolic Therapy Restrains In Vivo Ovarian Tumor Growth
Methylene Blue Metabolic Therapy Restrains In Vivo Ovarian Tumor Growth -
 Gender-Specific Genetic Predisposition to Breast Cancer: BRCA Genes and Beyond
Gender-Specific Genetic Predisposition to Breast Cancer: BRCA Genes and Beyond -
 The Role of the Complement in Clear Cell Renal Carcinoma (ccRCC)—What Future Prospects Are There for Its Use in Clinical Practice?
The Role of the Complement in Clear Cell Renal Carcinoma (ccRCC)—What Future Prospects Are There for Its Use in Clinical Practice? -
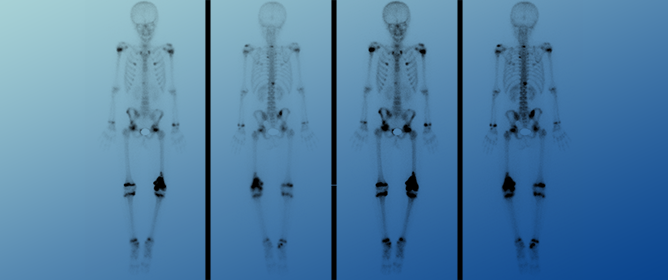 Primary Multi-Systemic Metastases in Osteosarcoma: Presentation, Treatment, and Survival of 83 Patients of the Cooperative Osteosarcoma Study Group
Primary Multi-Systemic Metastases in Osteosarcoma: Presentation, Treatment, and Survival of 83 Patients of the Cooperative Osteosarcoma Study Group -
 Addressing Genetic Tumor Heterogeneity, Post-Therapy Metastatic Spread, Cancer Repopulation, and Development of Acquired Tumor Cell Resistance
Addressing Genetic Tumor Heterogeneity, Post-Therapy Metastatic Spread, Cancer Repopulation, and Development of Acquired Tumor Cell Resistance
Journal Description
Cancers
Cancers
is a peer-reviewed, open access journal of oncology, published semimonthly online by MDPI. The Irish Association for Cancer Research (IACR), Spanish Association for Cancer Research (ASEICA), Biomedical Research Centre (CIBM), British Neuro-Oncology Society (BNOS) and Spanish Group for Cancer Immuno-Biotherapy (GÉTICA) are affiliated with Cancers and their members receive a discount on the article processing charges.
- Open Access— free for readers, with article processing charges (APC) paid by authors or their institutions.
- High Visibility: indexed within Scopus, SCIE (Web of Science), PubMed, PMC, Embase, CAPlus / SciFinder, and other databases.
- Journal Rank: JCR - Q2 (Oncology) / CiteScore - Q1 (Oncology)
- Rapid Publication: manuscripts are peer-reviewed and a first decision is provided to authors approximately 17.9 days after submission; acceptance to publication is undertaken in 2.8 days (median values for papers published in this journal in the second half of 2023).
- Recognition of Reviewers: reviewers who provide timely, thorough peer-review reports receive vouchers entitling them to a discount on the APC of their next publication in any MDPI journal, in appreciation of the work done.
- Sections: published in 18 topical sections.
- Companion journals for Cancers include: Radiation and Onco.
Impact Factor:
5.2 (2022);
5-Year Impact Factor:
5.6 (2022)
Latest Articles
Implementation of Artificial Intelligence in Personalized Prognostic Assessment of Lung Cancer: A Narrative Review
Cancers 2024, 16(10), 1832; https://doi.org/10.3390/cancers16101832 (registering DOI) - 10 May 2024
Abstract
Artificial Intelligence (AI) has revolutionized the management of non-small-cell lung cancer (NSCLC) by enhancing different aspects, including staging, prognosis assessment, treatment prediction, response evaluation, recurrence/prognosis prediction, and personalized prognostic assessment. AI algorithms may accurately classify NSCLC stages using machine learning techniques and deep
[...] Read more.
Artificial Intelligence (AI) has revolutionized the management of non-small-cell lung cancer (NSCLC) by enhancing different aspects, including staging, prognosis assessment, treatment prediction, response evaluation, recurrence/prognosis prediction, and personalized prognostic assessment. AI algorithms may accurately classify NSCLC stages using machine learning techniques and deep imaging data analysis. This could potentially improve precision and efficiency in staging, facilitating personalized treatment decisions. Furthermore, there are data suggesting the potential application of AI-based models in predicting prognosis in terms of survival rates and disease progression by integrating clinical, imaging and molecular data. In the present narrative review, we will analyze the preliminary studies reporting on how AI algorithms could predict responses to various treatment modalities, such as surgery, radiotherapy, chemotherapy, targeted therapy, and immunotherapy. There is robust evidence suggesting that AI also plays a crucial role in predicting the likelihood of tumor recurrence after surgery and the pattern of failure, which has significant implications for tailoring adjuvant treatments. The successful implementation of AI in personalized prognostic assessment requires the integration of different data sources, including clinical, molecular, and imaging data. Machine learning (ML) and deep learning (DL) techniques enable AI models to analyze these data and generate personalized prognostic predictions, allowing for a precise and individualized approach to patient care. However, challenges relating to data quality, interpretability, and the ability of AI models to generalize need to be addressed. Collaboration among clinicians, data scientists, and regulators is critical for the responsible implementation of AI and for maximizing its benefits in providing a more personalized prognostic assessment. Continued research, validation, and collaboration are essential to fully exploit the potential of AI in NSCLC management and improve patient outcomes. Herein, we have summarized the state of the art of applications of AI in lung cancer for predicting staging, prognosis, and pattern of recurrence after treatment in order to provide to the readers a large comprehensive overview of this challenging issue.
Full article
(This article belongs to the Special Issue Innovative Prognostic Factors and Follow-Up of Localized Thoracic Malignancies)
Open AccessReview
Insights in Molecular Therapies for Hepatocellular Carcinoma
by
Philipp Heumann, Andreas Albert, Karsten Gülow, Deniz Tümen, Martina Müller and Arne Kandulski
Cancers 2024, 16(10), 1831; https://doi.org/10.3390/cancers16101831 (registering DOI) - 10 May 2024
Abstract
We conducted a comprehensive review of the current literature of published data and clinical trials (MEDLINE), as well as published congress contributions and active recruiting clinical trials on targeted therapies in hepatocellular carcinoma. Combinations of different agents and medical therapy along with radiological
[...] Read more.
We conducted a comprehensive review of the current literature of published data and clinical trials (MEDLINE), as well as published congress contributions and active recruiting clinical trials on targeted therapies in hepatocellular carcinoma. Combinations of different agents and medical therapy along with radiological interventions were analyzed for the setting of advanced HCC. Those settings were also analyzed in combination with adjuvant situations after resection or radiological treatments. We summarized the current knowledge for each therapeutic setting and combination that currently is or has been under clinical evaluation. We further discuss the results in the background of current treatment guidelines. In addition, we review the pathophysiological mechanisms and pathways for each of these investigated targets and drugs to further elucidate the molecular background and underlying mechanisms of action. Established and recommended targeted treatment options that already exist for patients are considered for systemic treatment: atezolizumab/bevacizumab, durvalumab/tremelimumab, sorafenib, lenvatinib, cabozantinib, regorafenib, and ramucirumab. Combination treatment for systemic treatment and local ablative treatment or transarterial chemoembolization and adjuvant and neoadjuvant treatment strategies are under clinical investigation.
Full article
(This article belongs to the Section Molecular Cancer Biology)
Open AccessReview
Advances in Hodgkin Lymphoma Treatment: From Molecular Biology to Clinical Practice
by
Corrado Benevolo Savelli, Matteo Bisio, Luca Legato, Filippo Fasano, Elisa Santambrogio, Maura Nicolosi, Deborah Morra, Carola Boccomini, Roberto Freilone, Barbara Botto and Mattia Novo
Cancers 2024, 16(10), 1830; https://doi.org/10.3390/cancers16101830 (registering DOI) - 10 May 2024
Abstract
Classical Hodgkin Lymphoma (cHL) is a highly curable disease, but around 20% of patients experience progression or relapse after standard frontline chemotherapy regimens. Salvage regimens followed by autologous stem cell transplants represent the historical treatment approach for these cases. In the last decade,
[...] Read more.
Classical Hodgkin Lymphoma (cHL) is a highly curable disease, but around 20% of patients experience progression or relapse after standard frontline chemotherapy regimens. Salvage regimens followed by autologous stem cell transplants represent the historical treatment approach for these cases. In the last decade, with the increasing understanding of cHL biology and tumor microenvironment role in disease course, novel molecules have been introduced in clinical practice, improving outcomes in the relapsed/refractory setting. The anti-CD30 antibody-drug conjugated brentuximab vedotin and PD-1/PD-L1 checkpoint inhibitors represent nowadays curative options for chemorefractory patients, and randomized trials recently demonstrated their efficacy in frontline immune-chemo-combined modalities. Several drugs able to modulate the patients’ T-lymphocytes and NK cell activity are under development, as well as many anti-CD30 chimeric antigen receptor T-cell products. Multiple tumor aberrant epigenetic mechanisms are being investigated as targets for antineoplastic compounds such as histone deacetylase inhibitors and hypomethylating agents. Moreover, JAK2 inhibition combined with anti-PD1 blockade revealed a potential complementary therapeutic pathway in cHL. In this review, we will summarize recent findings on cHL biology and novel treatment options clinically available, as well as promising future perspectives in the field.
Full article
(This article belongs to the Special Issue Hodgkin Lymphoma (Volume II))
Open AccessArticle
Incidence of Pediatric Cancers in French Guiana: How Does It Compare to Global Estimates?
by
Mathieu Nacher, Qiannan Wang, Lindsay Osei, Benjamin Faivre, Narcisse Elenga, Antoine Adenis, Nathalie Deschamps and Kinan Drak Alsibai
Cancers 2024, 16(10), 1829; https://doi.org/10.3390/cancers16101829 (registering DOI) - 10 May 2024
Abstract
French Guiana is a French territory in South America. The exposome of persons living there is quite different from that in mainland France and the ethnic make-up of the population is also quite different. Poverty is also widespread with difficulties in accessing care
[...] Read more.
French Guiana is a French territory in South America. The exposome of persons living there is quite different from that in mainland France and the ethnic make-up of the population is also quite different. Poverty is also widespread with difficulties in accessing care magnified by the low medical-professional density. In this singular context, we aimed to measure the incidence of pediatric cancers and to compare it with other continents. We used French Guiana’s certified cancer registry to study this between 2003 and 2017. Incidences were standardized using the world population with three strata: 0–4 years, 5–9 years, and 10–14 years. There were 164 solid tumors or hematologic malignancies diagnosed in children under the age of 15 (92 in boys and 72 in girls). Over the study period, the standardized incidence rate was 14.1 per 100,000 among children aged under 15 years. There was no significant trend during the study period. The three most common causes of cancer were leukemias—mostly lymphoblastic—CNS tumors, and sarcoma. The standardized incidence of pediatric cancers in French Guiana was similar to those in Western Europe and North America. As others have discovered, we found that males tended to be more likely to develop cancer, notably leukemia, CNS tumors, sarcoma, and retinoblastoma. As elsewhere, the predominant cancer types changed with age. Our initial assumption was that given the singular context of French Guiana, there may have been differences in pediatric cancer incidences. Here we showed that overall, contrary to our assumption and to trends in tropical countries, the incidence of pediatric cancers was in a range between Western Europe and North America with some apparent but non-significant differences in the main types of cancers observed in global statistics. Quality cancer registry data in this tropical region confirm the suspicion that lower incidences in tropical low- and middle-income countries are likely to result from incomplete diagnosis and data collection.
Full article
(This article belongs to the Section Pediatric Oncology)
Open AccessArticle
Abemaciclib for the Treatment of HR+HER2− Metastatic Breast Cancer: An Institutional Experience
by
Erika Matos, Kaja Cankar, Neža Režun, Katja Dejanović and Tanja Ovčariček
Cancers 2024, 16(10), 1828; https://doi.org/10.3390/cancers16101828 (registering DOI) - 10 May 2024
Abstract
(1) Background: Abemaciclib combined with endocrine therapy is a standard first- or later--line of treatment for HR+/HER2− metastatic breast cancer (MBC). The aim of this retrospective cohort study was to describe the outcomes of patients treated in a real-world setting, with particular focus
[...] Read more.
(1) Background: Abemaciclib combined with endocrine therapy is a standard first- or later--line of treatment for HR+/HER2− metastatic breast cancer (MBC). The aim of this retrospective cohort study was to describe the outcomes of patients treated in a real-world setting, with particular focus on elderly patients. (2) Patients and methods: Patients treated with abemaciclib between November 2019 and February 2022 were included in the study. Data were collected from electronic medical records. The primary objective was to determine real-world progression-free survival (rwPFS), and secondary objectives included median overall survival (mOS) and safety. (3) Results: Analysis included 134 patients, with a median follow-up of 42 months. Median age was 62 years, with 29.9% aged 70+ years. A total of 51.5% of patients received abemaciclib in first-line, predominantly with aromatase inhibitor (68.1%). Median rwPFS was 21 in first-line and 20 months in the second-line, with no significant difference between treatment lines (HR 0.96; p = 0.88). Patients treated in the third- or later-line had a significantly shorter rwPFS, at 7 months (HR 1.48, p = 0.003). mOS was not reached in the first-line setting. For second- and third- or later-lines, mOS was 29 and 19 months, respectively. There was no significant difference in mOS between first- or second-line (HR 1.37, p = 0.36). In the 70+ group, median rwPFS was 15 months and mOS was 25 months with no significant difference compared to younger patients (rwPFS HR 1.1; p = 0.65; OS HR 1.4; p = 0.21). Most common adverse events (AEs) were diarrhoea (68.7%), anaemia (64.9%), and increased serum creatinine (63.4%). Grade 3/4 AEs were reported in 21.6% of patients. Dose reductions occurred in 30.6% of patients and were more frequent in patients 70+ (40%) compared to younger patients (28%); the difference was not significant (p = 0.22). At study cut-off, 64.9% of patients discontinued abemaciclib, primarily due to disease progression (73.5%). (4) Conclusions: Our study provides valuable insights into the effectiveness and safety of abemaciclib for the treatment of MBC. We observed comparable outcomes in terms of rwPFS and OS between the first two lines, suggesting consistent effectiveness across treatment lines. In addition, our findings suggest that older age (70+) does not significantly impact the effectiveness and tolerability of abemaciclib, although the careful monitoring and management of AEs are warranted.
Full article
(This article belongs to the Section Clinical Research of Cancer)
Open AccessArticle
Speeding Up and Improving Image Quality in Glioblastoma MRI Protocol by Deep Learning Image Reconstruction
by
Georg Gohla, Till-Karsten Hauser, Paula Bombach, Daniel Feucht, Arne Estler, Antje Bornemann, Leonie Zerweck, Eliane Weinbrenner, Ulrike Ernemann and Christer Ruff
Cancers 2024, 16(10), 1827; https://doi.org/10.3390/cancers16101827 (registering DOI) - 10 May 2024
Abstract
A fully diagnostic MRI glioma protocol is key to monitoring therapy assessment but is time-consuming and especially challenging in critically ill and uncooperative patients. Artificial intelligence demonstrated promise in reducing scan time and improving image quality simultaneously. The purpose of this study was
[...] Read more.
A fully diagnostic MRI glioma protocol is key to monitoring therapy assessment but is time-consuming and especially challenging in critically ill and uncooperative patients. Artificial intelligence demonstrated promise in reducing scan time and improving image quality simultaneously. The purpose of this study was to investigate the diagnostic performance, the impact on acquisition acceleration, and the image quality of a deep learning optimized glioma protocol of the brain. Thirty-three patients with histologically confirmed glioblastoma underwent standardized brain tumor imaging according to the glioma consensus recommendations on a 3-Tesla MRI scanner. Conventional and deep learning-reconstructed (DLR) fluid-attenuated inversion recovery, and T2- and T1-weighted contrast-enhanced Turbo spin echo images with an improved in-plane resolution, i.e., super-resolution, were acquired. Two experienced neuroradiologists independently evaluated the image datasets for subjective image quality, diagnostic confidence, tumor conspicuity, noise levels, artifacts, and sharpness. In addition, the tumor volume was measured in the image datasets according to Response Assessment in Neuro-Oncology (RANO) 2.0, as well as compared between both imaging techniques, and various clinical–pathological parameters were determined. The average time saving of DLR sequences was 30% per MRI sequence. Simultaneously, DLR sequences showed superior overall image quality (all p < 0.001), improved tumor conspicuity and image sharpness (all p < 0.001, respectively), and less image noise (all p < 0.001), while maintaining diagnostic confidence (all p > 0.05), compared to conventional images. Regarding RANO 2.0, the volume of non-enhancing non-target lesions (p = 0.963), enhancing target lesions (p = 0.993), and enhancing non-target lesions (p = 0.951) did not differ between reconstruction types. The feasibility of the deep learning-optimized glioma protocol was demonstrated with a 30% reduction in acquisition time on average and an increased in-plane resolution. The evaluated DLR sequences improved subjective image quality and maintained diagnostic accuracy in tumor detection and tumor classification according to RANO 2.0.
Full article
(This article belongs to the Special Issue Artificial Intelligence and Deep Learning in Radiology Oncology)
►▼
Show Figures

Figure 1
Open AccessEditorial
Up to the Herculean Task of Tackling Cancer Therapy Resistance
by
Kostas A. Papavassiliou and Athanasios G. Papavassiliou
Cancers 2024, 16(10), 1826; https://doi.org/10.3390/cancers16101826 (registering DOI) - 10 May 2024
Abstract
Cancer therapy resistance still poses the biggest hurdle to cancer treatment...[]
Full article
(This article belongs to the Section Cancer Pathophysiology)
Open AccessArticle
Efficacy of Pembrolizumab vs. Nivolumab Plus Ipilimumab in Metastatic NSCLC in Relation to PD-L1 and TMB Status
by
Walid Shalata, Natalie Maimon Rabinovich, Abed Agbarya, Alexander Yakobson, Yulia Dudnik, Ashraf Abu Jama, Ahron Yehonatan Cohen, Sondos Shalata, Ahmad Abu Hamed, Tahel Ilan Ber, Oshri Machluf, Gal Shoham Levin and Amichay Meirovitz
Cancers 2024, 16(10), 1825; https://doi.org/10.3390/cancers16101825 (registering DOI) - 10 May 2024
Abstract
The efficacy of immune checkpoint inhibitor (ICI) therapy concerning programmed death ligand 1 (PD-L1) status is well established in patients diagnosed with non-small cell lung cancer (NSCLC). However, there remains a paucity of evidence regarding the efficacy concerning tumor mutational burden (TMB) in
[...] Read more.
The efficacy of immune checkpoint inhibitor (ICI) therapy concerning programmed death ligand 1 (PD-L1) status is well established in patients diagnosed with non-small cell lung cancer (NSCLC). However, there remains a paucity of evidence regarding the efficacy concerning tumor mutational burden (TMB) in both clinical trials and real-world data (RWD). In the current article, clinicopathological and molecular epidemiological data were meticulously collected, and treatment modalities were meticulously recorded. The final analysis included a study population of 194 patients. Median age was 67 years (range 37–86), with the majority being male (71.13%), and 85.71% of patients were either current or former smokers at diagnosis. Adenocarcinoma accounted for most diagnoses (71.65%), followed by squamous cell carcinoma (24.23%). In terms of PD-L1 status, 42.78% had an expression level below 1%, 28.35% had an expression between 1–49%, and 28.87% had an expression above 50%. The TMB ranged from 0 to 75, with a median of 10.31 (range 0–75) for PD-L1 expression below 1%, with a median of 9.73 (range 0.95–39.63) for PD-L1 expression between 1–49%, and a median of 9.72 (range 0.95–48) for PD-L1 expression above 50%. Corresponding to patients with low PDL-1 less than 1% and low TMB (0–5), the median overall survival (mOS) was 16 (p = 0.18), and 15 months (p = 0.22), patients with medium PDL-1 (1–49%) and medium TMB (5–10), the mOS was 15 (p = 0.18) and 16 months (p = 0.22), patients with high PDL-1 (>50) and high TMB (>10), the mOS was 24 (p = 0.18) and 21 (p = 0.22) months. This study represents the largest academic RWD dataset concerning PD-L1 and TMB status in patients with locally advanced and metastatic NSCLC.
Full article
(This article belongs to the Section Cancer Metastasis)
Open AccessReview
Relapse Prevention in Acute Myeloid Leukemia: The Role of Immunotherapy with Histamine Dihydrochloride and Low-Dose Interleukin-2
by
Pau Montesinos, Francesco Buccisano, Thomas Cluzeau, Lovisa Vennström and Michael Heuser
Cancers 2024, 16(10), 1824; https://doi.org/10.3390/cancers16101824 (registering DOI) - 10 May 2024
Abstract
The treatment and management of acute myeloid leukemia (AML) has improved in recent decennia by targeted therapy for subgroups of patients, expanded indications for allogeneic stem cell transplantation (allo-SCT) and surveillance of residual or arising leukemia. However, hematological relapse among patients who have
[...] Read more.
The treatment and management of acute myeloid leukemia (AML) has improved in recent decennia by targeted therapy for subgroups of patients, expanded indications for allogeneic stem cell transplantation (allo-SCT) and surveillance of residual or arising leukemia. However, hematological relapse among patients who have attained complete remission (CR) after the initial courses of chemotherapy remains a significant cause of morbidity and mortality. Here, we review an immunotherapeutic option using histamine dihydrochloride and low-dose interleukin-2 (HDC/LD-IL-2) for remission maintenance in AML. The treatment is approved in Europe in the post-consolidation phase to avoid relapse among patients in CR who are not candidates for upfront allo-SCT. We present aspects of the purported anti-leukemic mechanism of this regimen, including translation of preclinical results into the clinical setting, along with relapse prevention in subgroups of patients. We consider that HDC/LD-IL-2 is a conceivable option for younger adults, in particular patients with AML of normal karyotype and those with favorable responses to the initial chemotherapy. HDC/LD-IL-2 may form an emerging landscape of remission maintenance in AML.
Full article
(This article belongs to the Topic Myeloma and Leukemia-Challenges and Current Treatment Options)
Open AccessArticle
Frequency of Common and Uncommon BRAF Alterations among Colorectal and Non-Colorectal Gastrointestinal Malignancies
by
Amit Mahipal, Michael H. Storandt, Emily A. Teslow, Ellen Jaeger, Melissa C. Stoppler, Zhaohui Jin and Sakti Chakrabarti
Cancers 2024, 16(10), 1823; https://doi.org/10.3390/cancers16101823 - 10 May 2024
Abstract
Background: The predictive and prognostic role of BRAF alterations has been evaluated in colorectal cancer (CRC); however, BRAF alterations have not been fully characterized in non-CRC gastrointestinal (GI) malignancies. In the present study, we report the frequency and spectrum of BRAF alterations among
[...] Read more.
Background: The predictive and prognostic role of BRAF alterations has been evaluated in colorectal cancer (CRC); however, BRAF alterations have not been fully characterized in non-CRC gastrointestinal (GI) malignancies. In the present study, we report the frequency and spectrum of BRAF alterations among patients with non-CRC GI malignancies. Methods: Patients with CRC and non-CRC GI malignancies who underwent somatic tumor profiling via a tissue-based or liquid-based assay were included in this study. Gain-of-function BRAF alterations were defined as pathogenic/likely pathogenic somatic short variants (SVs), copy number amplifications ≥8, or fusions (RNA or DNA). Results: Among 51,560 patients with somatic profiling, 40% had CRC and 60% had non-CRC GI malignancies. BRAF GOF alterations were seen more frequently in CRC (8.9%) compared to non-CRC GI malignancies (2.2%) (p < 0.001). Non-CRC GI malignancies with the highest prevalence of BRAF GOF alterations were bile duct cancers (4.1%) and small intestine cancers (4.0%). Among BRAF GOF alterations, class II (28% vs. 6.8%, p < 0.001) and class III (23% vs. 14%, p < 0.001) were more common in non-CRC GI malignancies. Among class II alterations, rates of BRAF amplifications (3.1% vs. 0.3%, p < 0.001) and BRAF fusions (12% vs. 2.2%, p < 0.001) were higher in non-CRC GI malignancies compared to CRC. Conclusions: Non-CRC GI malignancies demonstrate a distinct BRAF alteration profile compared to CRC, with a higher frequency of class II and III mutations, and more specifically, a higher incidence of BRAF fusions. Future studies should evaluate clinical implications for the management of non-CRC GI patients with BRAF alterations, especially BRAF fusions.
Full article
(This article belongs to the Special Issue Clinical and Pathologic Response to Therapy in Gastrointestinal Oncology)
►▼
Show Figures

Figure 1
Open AccessArticle
Autonomous Tumor Signature Extraction Applied to Spatially Registered Bi-Parametric MRI to Predict Prostate Tumor Aggressiveness: A Pilot Study
by
Rulon Mayer, Baris Turkbey and Charles B. Simone II
Cancers 2024, 16(10), 1822; https://doi.org/10.3390/cancers16101822 - 10 May 2024
Abstract
Background: Accurate, reliable, non-invasive assessment of patients diagnosed with prostate cancer is essential for proper disease management. Quantitative assessment of multi-parametric MRI, such as through artificial intelligence or spectral/statistical approaches, can provide a non-invasive objective determination of the prostate tumor aggressiveness without side
[...] Read more.
Background: Accurate, reliable, non-invasive assessment of patients diagnosed with prostate cancer is essential for proper disease management. Quantitative assessment of multi-parametric MRI, such as through artificial intelligence or spectral/statistical approaches, can provide a non-invasive objective determination of the prostate tumor aggressiveness without side effects or potential poor sampling from needle biopsy or overdiagnosis from prostate serum antigen measurements. To simplify and expedite prostate tumor evaluation, this study examined the efficacy of autonomously extracting tumor spectral signatures for spectral/statistical algorithms for spatially registered bi-parametric MRI. Methods: Spatially registered hypercubes were digitally constructed by resizing, translating, and cropping from the image sequences (Apparent Diffusion Coefficient (ADC), High B-value, T2) from 42 consecutive patients in the bi-parametric MRI PI-CAI dataset. Prostate cancer blobs exceeded a threshold applied to the registered set from normalizing the registered set into an image that maximizes High B-value, but minimizes the ADC and T2 images, appearing “green” in the color composite. Clinically significant blobs were selected based on size, average normalized green value, sliding window statistics within a blob, and position within the hypercube. The center of mass and maximized sliding window statistics within the blobs identified voxels associated with tumor signatures. We used correlation coefficients (R) and p-values, to evaluate the linear regression fits of the z-score and SCR (with processed covariance matrix) to tumor aggressiveness, as well as Area Under the Curves (AUC) for Receiver Operator Curves (ROC) from logistic probability fits to clinically significant prostate cancer. Results: The highest R (R > 0.45), AUC (>0.90), and lowest p-values (<0.01) were achieved using z-score and modified registration applied to the covariance matrix and tumor signatures selected from the “greenest” parts from the selected blob. Conclusions: The first autonomous tumor signature applied to spatially registered bi-parametric MRI shows promise for determining prostate tumor aggressiveness.
Full article
(This article belongs to the Section Methods and Technologies Development)
►▼
Show Figures

Figure 1
Open AccessArticle
Poor Mobilization-Associated Factors in Autologous Hematopoietic Stem Cell Harvest
by
Won Kee Ahn, Hyun-Jun Nam, Hae Won Lee, Seungmin Hahn, Jung Woo Han, Chuhl Joo Lyu, Sinyoung Kim, Soon Sung Kwon, Haerim Chung, Jin Seok Kim, June-Won Cheong and Kyung-A Lee
Cancers 2024, 16(10), 1821; https://doi.org/10.3390/cancers16101821 - 10 May 2024
Abstract
Peripheral blood stem cell transplantation (PBSCT) is an important therapeutic measure for both hematologic and non-hematologic diseases. For PBSCT to be successful, sufficient CD34+ cells need to be mobilized and harvested. Although risk factors associated with poor mobilization in patients with hematologic
[...] Read more.
Peripheral blood stem cell transplantation (PBSCT) is an important therapeutic measure for both hematologic and non-hematologic diseases. For PBSCT to be successful, sufficient CD34+ cells need to be mobilized and harvested. Although risk factors associated with poor mobilization in patients with hematologic diseases have been reported, studies of patients with non-hematologic diseases and those receiving plerixafor are rare. To identify factors associated with poor mobilization, data from autologous PBSC harvest (PBSCH) in 491 patients were retrospectively collected and analyzed. A multivariate analysis revealed that in patients with a hematologic disease, an age older than 60 years (odds ratio [OR] 1.655, 95% confidence interval [CI] 1.049–2.611, p = 0.008), the use of myelotoxic agents (OR 4.384, 95% CI 2.681–7.168, p < 0.001), and a low platelet count (OR 2.106, 95% CI 1.205–3.682, p = 0.009) were associated with poor mobilization. In patients with non-hematologic diseases, a history of radiation on the pelvis/spine was the sole associated factor (OR 12.200, 95% CI 1.934–76.956, p = 0.008). Among the group of patients who received plerixafor, poor mobilization was observed in 19 patients (19/134, 14.2%) and a difference in the mobilization regimen was noted among the good mobilization group. These results show that the risk factors for poor mobilization in patients with non-hematologic diseases and those receiving plerixafor differ from those in patients with hematologic diseases; as such, non-hematologic patients require special consideration to enable successful PBSCH.
Full article
(This article belongs to the Section Clinical Research of Cancer)
Open AccessReview
Updates on the Management of Colorectal Cancer in Older Adults
by
Conor D. J. O’Donnell, Joleen Hubbard and Zhaohui Jin
Cancers 2024, 16(10), 1820; https://doi.org/10.3390/cancers16101820 - 10 May 2024
Abstract
Colorectal cancer (CRC) poses a significant global health challenge. Notably, the risk of CRC escalates with age, with the majority of cases occurring in those over the age of 65. Despite recent progress in tailoring treatments for early and advanced CRC, there is
[...] Read more.
Colorectal cancer (CRC) poses a significant global health challenge. Notably, the risk of CRC escalates with age, with the majority of cases occurring in those over the age of 65. Despite recent progress in tailoring treatments for early and advanced CRC, there is a lack of prospective data to guide the management of older patients, who are frequently underrepresented in clinical trials. This article reviews the contemporary landscape of managing older individuals with CRC, highlighting recent advancements and persisting challenges. The role of comprehensive geriatric assessment is explored. Opportunities for treatment escalation/de-escalation, with consideration of the older adult’s fitness level. are reviewed in the neoadjuvant, surgical, adjuvant, and metastatic settings of colon and rectal cancers. Immunotherapy is shown to be an effective treatment option in older adults who have CRC with microsatellite instability. Promising new technologies such as circulating tumor DNA and recent phase III trials adding later-line systemic therapy options are discussed. Clinical recommendations based on the data available are summarized. We conclude that deliberate efforts to include older individuals in future colorectal cancer trials are essential to better guide the management of these patients in this rapidly evolving field.
Full article
(This article belongs to the Topic Advances in Colorectal Cancer Therapy)
Open AccessReview
FLT3-Mutated Leukemic Stem Cells: Mechanisms of Resistance and New Therapeutic Targets
by
Debora Capelli
Cancers 2024, 16(10), 1819; https://doi.org/10.3390/cancers16101819 - 10 May 2024
Abstract
Despite the availability of target drugs in the first and second line, only 30% of FLT3mut AMLs are cured. Among the multiple mechanisms of resistance, those of FLT3mut LSC are the most difficult to eradicate because of their metabolic and genomic characteristics. Reactivation
[...] Read more.
Despite the availability of target drugs in the first and second line, only 30% of FLT3mut AMLs are cured. Among the multiple mechanisms of resistance, those of FLT3mut LSC are the most difficult to eradicate because of their metabolic and genomic characteristics. Reactivation of glycogen synthesis, inhibition of the RAS/MAPK pathway, and degradation of FLT3 may be potential aids to fight the resistance of LSC to FLT3i. LSC is also characterized by the expression of a CD34+/CD25+/CD123+/CD99+ immunophenotype. The receptor and ligand of FLT3, the natural killer group 2 member D ligand (NKGD2L), and CD123 are some of the targets of chimeric antigen receptor T cells (CAR-T), bispecific T-cell engager molecules (BiTEs), CAR-NK and nanoparticles recently designed and reported here. The combination of these new therapeutic options, hopefully in a minimal residual disease (MRD)-driven approach, could provide the future answer to the challenge of treating FLT3mut AML.
Full article
(This article belongs to the Special Issue The New Challenge of Curing AML: Analysis of Mechanisms of Resistance of Target Drugs and Future Perspectives)
►▼
Show Figures

Figure 1
Open AccessArticle
LKB1 Loss Correlates with STING Loss and, in Cooperation with β-Catenin Membranous Loss, Indicates Poor Prognosis in Patients with Operable Non-Small Cell Lung Cancer
by
Eleni D. Lagoudaki, Anastasios V. Koutsopoulos, Maria Sfakianaki, Chara Papadaki, Georgios C. Manikis, Alexandra Voutsina, Maria Trypaki, Eleftheria Tsakalaki, Georgia Fiolitaki, Dora Hatzidaki, Emmanuel Yiachnakis, Dimitra Koumaki, Dimitrios Mavroudis, Maria Tzardi, Efstathios N. Stathopoulos, Kostas Marias, Vassilis Georgoulias and John Souglakos
Cancers 2024, 16(10), 1818; https://doi.org/10.3390/cancers16101818 - 10 May 2024
Abstract
To investigate the incidence and prognostically significant correlations and cooperations of LKB1 loss of expression in non-small cell lung cancer (NSCLC), surgical specimens from 188 metastatic and 60 non-metastatic operable stage I-IIIA NSCLC patients were analyzed to evaluate their expression of LKB1 and
[...] Read more.
To investigate the incidence and prognostically significant correlations and cooperations of LKB1 loss of expression in non-small cell lung cancer (NSCLC), surgical specimens from 188 metastatic and 60 non-metastatic operable stage I-IIIA NSCLC patients were analyzed to evaluate their expression of LKB1 and pAMPK proteins in relation to various processes. The investigated factors included antitumor immunity response regulators STING and PD-L1; pro-angiogenic, EMT and cell cycle targets, as well as metastasis-related (VEGFC, PDGFRα, PDGFRβ, p53, p16, Cyclin D1, ZEB1, CD24) targets; and cell adhesion (β-catenin) molecules. The protein expression levels were evaluated via immunohistochemistry; the RNA levels of LKB1 and NEDD9 were evaluated via PCR, while KRAS exon 2 and BRAFV600E mutations were evaluated by Sanger sequencing. Overall, loss of LKB1 protein expression was observed in 21% (51/248) patients and correlated significantly with histotype (p < 0.001), KRAS mutations (p < 0.001), KC status (concomitant KRAS mutation and p16 downregulation) (p < 0.001), STING loss (p < 0.001), and high CD24 expression (p < 0.001). STING loss also correlated significantly with loss of LKB1 expression in the metastatic setting both overall (p = 0.014) and in lung adenocarcinomas (LUACs) (p = 0.005). Additionally, LKB1 loss correlated significantly with a lack of or low β-catenin membranous expression exclusively in LUACs, both independently of the metastatic status (p = 0.019) and in the metastatic setting (p = 0.007). Patients with tumors yielding LKB1 loss and concomitant nonexistent or low β-catenin membrane expression experienced significantly inferior median overall survival of 20.50 vs. 52.99 months; p < 0.001 as well as significantly greater risk of death (HR: 3.32, 95% c.i.: 1.71–6.43; p <0.001). Our findings underscore the impact of the synergy of LKB1 with STING and β-catenin in NSCLC, in prognosis.
Full article
(This article belongs to the Special Issue Advancements in Lung Cancer Surgical Treatment and Prognosis)
►▼
Show Figures

Figure 1
Open AccessArticle
Ki67 Tumor Expression Predicts Treatment Benefit Achieved by Macroscopic Radical Lung-Preserving Surgery in Pleural Mesothelioma—A Retrospective Multicenter Analysis
by
Sarah Hintermair, Stephanie Iser, Alexander Varga, Melanie Biesinger, Tomas Bohanes, Ali Celik, Muhammet Sayan, Aykut Kankoç, Nalan Akyurek, Betul Öğüt, Elisabeth Stubenberger and Bahil Ghanim
Cancers 2024, 16(10), 1817; https://doi.org/10.3390/cancers16101817 - 10 May 2024
Abstract
Pleural mesothelioma (PM), linked to asbestos-induced inflammation, carries a poor prognosis. Therapy ranges from therapy limitation to aggressive multimodality treatment. Given the uncertainty about treatment benefits for patients, this study aimed to assess the role of Ki67 as a prognostic and predictive parameter
[...] Read more.
Pleural mesothelioma (PM), linked to asbestos-induced inflammation, carries a poor prognosis. Therapy ranges from therapy limitation to aggressive multimodality treatment. Given the uncertainty about treatment benefits for patients, this study aimed to assess the role of Ki67 as a prognostic and predictive parameter in PM. Ki67 was measured in the specimens of 70 PM patients (17 female, 53 male) from two centers and correlated to overall survival (OS) and therapy outcome. The median OS was 16.1 months. The level of Ki67 expression was divided into low (≤15%) and high (>15%). A low value of Ki67 expression was associated with a longer OS (Ki67 ≤ 15%: 31.2 (95% CI 6.5–55.8) months vs. Ki67 > 15%: 11.1 (95% CI 7.7–14.6) months, p = 0.012). The 5-year survival represents 22% in the low Ki67 expression group, in contrast to 5% in the high Ki67 expression group. We found a significant interaction term of Ki67 with multimodality treatment (p = 0.031) translating to an OS of 48.1 months in the low expression Ki67 group compared to 24.3 months in the high Ki67 expression group when receiving surgery within multimodality therapy. Therefore, Ki67 stands out as a validated prognostic and, most importantly, novel predictive biomarker for treatment benefits, particularly regarding surgery within multimodality therapy.
Full article
(This article belongs to the Special Issue Recent Research on Mesothelioma)
►▼
Show Figures

Figure 1
Open AccessArticle
Extended Genotyping to Stratify the Risk of CIN2+ in Women with Persistent HPV Infection, Negative Cytology and Type 3 Transformation Zone
by
Maria Teresa Bruno, Gaetano Valenti, Antonino Giovanni Cavallaro, Ilenia Palermo, Tiziana Aiello, Jessica Farina, Marco Marzio Panella and Liliana Mereu
Cancers 2024, 16(10), 1816; https://doi.org/10.3390/cancers16101816 - 10 May 2024
Abstract
Persistent human papillomavirus (HPV) infection is recognized as a major risk factor for cervical cancer. Women with persistent HPV and negative cytology are at greater risk of CIN2+ than women with negative infection. The diagnosis becomes more complicated when the woman has a
[...] Read more.
Persistent human papillomavirus (HPV) infection is recognized as a major risk factor for cervical cancer. Women with persistent HPV and negative cytology are at greater risk of CIN2+ than women with negative infection. The diagnosis becomes more complicated when the woman has a type 3 transformation zone at colposcopy. The aim of this study was to determine the prevalence of CIN2+ in women with persistent HPV, negative cytology and TZ3; how to stratify the risk of CIN2+; and what the best diagnostic strategy is, given TZ3. Methods: In a multicenter retrospective cohort study, we enrolled women with negative cytology and TZ3 among the 213 women referred for colposcopy for persistent HPV. The average age of the women was 53 years; in particular, 83% were postmenopausal women. In the presence of a TZ3, the entire transformation zone cannot be explored, making colposcopy and targeted biopsy useless and inadequate, with great risks of underdiagnosis or missed diagnosis. Women with TZ3 underwent diagnostic LEEP to ensure correct diagnoses. Results: The study highlighted 19% (16/84) of CIN2+ lesions, a higher frequency of non-HPV 16/18 genotypes (76.2%), and 50% of CIN2+ lesions being due to non-HPV 16/18 genotypes. Furthermore, more than half of the women (80.9%) had normal histopathological results in the LEEP sample. Conclusion. Women with viral persistence, negative cytology, and TZ3 have a 19% risk of CIN2+; genotyping helps stratify risk, but extensive genotyping is necessary instead of partial genotyping (16/18), referring to a population of women over 50 years old in which the prevalence of genotypes 16,18 decreases and the prevalence of other genotypes increases; diagnostic LEEP is excessive (only 16 cases of CIN2+ out of 48 cases treated), even though 83% of women had viral clearance after LEEP; p16/Ki67 double staining could be a potential risk marker, which would only highlight women at risk of CIN2+ to undergo LEEP. To individualize the diagnostic workup and treatment and minimize the risk of under diagnosis and overtreatment, future studies should explore the use of extended genotyping and new biomarkers for individual risk stratification.
Full article
(This article belongs to the Section Cancer Causes, Screening and Diagnosis)
►▼
Show Figures

Figure 1
Open AccessArticle
Magnetic-Resonance-Imaging-Guided Cryoablation for Solitary-Biopsy-Proven Renal Cell Carcinoma: A Tertiary Cancer Center Experience
by
Mohamed E. Abdelsalam, Nabeel Mecci, Ahmed Awad, Roland L. Bassett, Bruno C. Odisio, Peiman Habibollahi, Thomas Lu, David Irwin, Jose A. Karam, Surena F. Matin and Kamran Ahrar
Cancers 2024, 16(10), 1815; https://doi.org/10.3390/cancers16101815 - 10 May 2024
Abstract
Background: Our purpose is to evaluate the long-term oncologic efficacy and survival rates of MRI-guided cryoablation for patients with biopsy-proven cT1a renal cell carcinoma (RCC). Materials and Methods: We retrospectively reviewed our renal ablation database between January 2007 and June 2021 and only
[...] Read more.
Background: Our purpose is to evaluate the long-term oncologic efficacy and survival rates of MRI-guided cryoablation for patients with biopsy-proven cT1a renal cell carcinoma (RCC). Materials and Methods: We retrospectively reviewed our renal ablation database between January 2007 and June 2021 and only included patients with solitary-biopsy-proven cT1a RCC (≤4 cm) who underwent MRI-guided cryoablation. We excluded patients with genetic syndromes, bilateral RCC, recurrent RCC or benign lesions, those without pathologically proven RCC lesions and patients who underwent radiofrequency ablation or CT-guided cryoablation. For each patient, we collected the following: age, sex, lesion size, right- or left-sided, pathology, ablation zone tumor recurrence, development of new tumor in the kidney other than ablation zone, development of metastatic disease, patient alive or not, date and cause of death. We used the Kaplan and Meier product limit estimator to estimate the survival outcomes. Results: Twenty-nine patients (median age 70 years) met our inclusion criteria. Twenty-nine MRI-guided cryoablation procedures were performed for twenty-nine tumor lesions with a median size of 2.2 cm. A Clavien–Dindo grade III complication developed in one patient (3.4%). Clear cell RCC was the most reported histology (n = 19). The median follow up was 4.5 years. No tumor recurrence or metastatic disease developed in any of the patients. Two patients developed new renal lesions separate from the ablation zone. The 5- and 10-year OS were 72% and 55.6%, respectively. The 5- and 10-year DFS were 90.5% and the 5-year and 10-year LRFS, MFS and CSS were all 100%. Conclusions: MRI-guided cryoablation is a safe treatment with a low complication rate. Long-term follow-up data revealed long-standing oncologic control.
Full article
(This article belongs to the Special Issue Genitourinary Malignancies)
►▼
Show Figures

Figure 1
Open AccessReview
Pediatric Diffuse Midline Glioma H3K27-Altered: From Developmental Origins to Therapeutic Challenges
by
Manuela Mandorino, Ahana Maitra, Domenico Armenise, Olga Maria Baldelli, Morena Miciaccia, Savina Ferorelli, Maria Grazia Perrone and Antonio Scilimati
Cancers 2024, 16(10), 1814; https://doi.org/10.3390/cancers16101814 - 10 May 2024
Abstract
Diffuse intrinsic pontine glioma (DIPG), now referred to as diffuse midline glioma (DMG), is a highly aggressive pediatric cancer primarily affecting children aged 4 to 9 years old. Despite the research and clinical trials conducted to identify a possible treatment for DIPG, no
[...] Read more.
Diffuse intrinsic pontine glioma (DIPG), now referred to as diffuse midline glioma (DMG), is a highly aggressive pediatric cancer primarily affecting children aged 4 to 9 years old. Despite the research and clinical trials conducted to identify a possible treatment for DIPG, no effective drug is currently available. These tumors often affect deep midline brain structures in young children, suggesting a connection to early brain development’s epigenetic regulation targets, possibly affecting neural progenitor functions and differentiation. The H3K27M mutation is a known DIPG trigger, but the exact mechanisms beyond epigenetic regulation remain unclear. After thoroughly examining the available literature, we found that over 85% of DIPG tumors contain a somatic missense mutation, K27M, in genes encoding histone H3.3 and H3.1, leading to abnormal gene expression that drives tumor growth and spread. This mutation impacts crucial brain development processes, including the epithelial–mesenchymal transition (EMT) pathway, and may explain differences between H3K27M and non-K27M pediatric gliomas. Effects on stem cells show increased proliferation and disrupted differentiation. The genomic organization of H3 gene family members in the developing brain has revealed variations in their expression patterns. All these observations suggest a need for global efforts to understand developmental origins and potential treatments.
Full article
(This article belongs to the Topic From Basic Research to a Clinical Perspective in Oncology)
►▼
Show Figures

Figure 1
Open AccessArticle
Resection Ratios and Tumor Eccentricity in Breast-Conserving Surgery Specimens for Surgical Accuracy Assessment
by
Dinusha Veluponnar, Behdad Dashtbozorg, Marcos Da Silva Guimaraes, Marie-Jeanne T. F. D. Vrancken Peeters, Lisanne L. de Boer and Theo J. M. Ruers
Cancers 2024, 16(10), 1813; https://doi.org/10.3390/cancers16101813 - 9 May 2024
Abstract
This study aims to evaluate several defined specimen parameters that would allow to determine the surgical accuracy of breast-conserving surgeries (BCS) in a representative population of patients. These specimen parameters could be used to compare surgical accuracy when using novel technologies for intra-operative
[...] Read more.
This study aims to evaluate several defined specimen parameters that would allow to determine the surgical accuracy of breast-conserving surgeries (BCS) in a representative population of patients. These specimen parameters could be used to compare surgical accuracy when using novel technologies for intra-operative BCS guidance in the future. Different specimen parameters were determined among 100 BCS patients, including the ratio of specimen volume to tumor volume (resection ratio) with different optimal margin widths (0 mm, 1 mm, 2 mm, and 10 mm). Furthermore, the tumor eccentricity [maximum tumor-margin distance − minimum tumor-margin distance] and the relative tumor eccentricity [tumor eccentricity ÷ pathological tumor diameter] were determined. Different patient subgroups were compared using Wilcoxon rank sum tests. When using a surgical margin width of 0 mm, 1 mm, 2 mm, and 10 mm, on average, 19.16 (IQR 44.36), 9.94 (IQR 18.09), 6.06 (IQR 9.69) and 1.35 (IQR 1.78) times the ideal resection volume was excised, respectively. The median tumor eccentricity among the entire patient population was 11.29 mm (SD = 3.99) and the median relative tumor eccentricity was 0.66 (SD = 2.22). Resection ratios based on different optimal margin widths (0 mm, 1 mm, 2 mm, and 10 mm) and the (relative) tumor eccentricity could be valuable outcome measures to evaluate the surgical accuracy of novel technologies for intra-operative BCS guidance.
Full article
(This article belongs to the Special Issue Recent Advances and Challenges in Breast Cancer Surgery)
►▼
Show Figures

Figure 1

Journal Menu
► ▼ Journal Menu-
- Cancers Home
- Aims & Scope
- Editorial Board
- Reviewer Board
- Topical Advisory Panel
- Instructions for Authors
- Special Issues
- Topics
- Sections & Collections
- Article Processing Charge
- Indexing & Archiving
- Editor’s Choice Articles
- Most Cited & Viewed
- Journal Statistics
- Journal History
- Journal Awards
- Society Collaborations
- Conferences
- Editorial Office
Journal Browser
► ▼ Journal BrowserHighly Accessed Articles
Latest Books
E-Mail Alert
News
Topics
Topic in
Bioengineering, Biomolecules, Cancers, Diseases, Nanomaterials, Pharmaceutics
Dynamic Nano-Biomaterials in Tissue Regeneration and Cancer Therapies
Topic Editors: Ramar Thangam, Heemin Kang, Bibin G. Anand, Ramachandran Vijayan, Venugopal KrishnanDeadline: 15 May 2024
Topic in
Biomedicines, Cancers, JFB, Nanomaterials, Polymers
Advanced Functional Materials for Regenerative Medicine
Topic Editors: Antonino Morabito, Luca ValentiniDeadline: 6 June 2024
Topic in
Biology, Cancers, Current Oncology, Diseases, JCM, Pathogens
Pathogenetic, Diagnostic and Therapeutic Perspectives in Head and Neck Cancer
Topic Editors: Shun-Fa Yang, Ming-Hsien ChienDeadline: 20 June 2024
Topic in
Cancers, Cells, JCM, Radiation, Pharmaceutics, Applied Sciences, Nanomaterials, Current Oncology
Innovative Radiation Therapies
Topic Editors: Gérard Baldacchino, Eric Deutsch, Marie Dutreix, Sandrine Lacombe, Erika Porcel, Charlotte Robert, Emmanuelle Bourneuf, João Santos Sousa, Aurélien de la LandeDeadline: 30 June 2024

Conferences
Special Issues
Special Issue in
Cancers
Molecular and Cellular Heterogeneity in an Evolving Tumor Landscape: When Diversity Gives Rise to Aggressive and Drug Resistant Cells
Guest Editor: Michelle R. DawsonDeadline: 20 May 2024
Special Issue in
Cancers
Innovations in Soft Tissue Sarcoma Diagnosis and Treatment
Guest Editors: Erlinda M. Gordon, Sant P. Chawla, Frederick L. HallDeadline: 30 May 2024
Special Issue in
Cancers
Perioperative Care and Pain Management in Cancer Patients: From Basic Science to Clinical Practice
Guest Editors: Dario Bugada, Juan P. CataDeadline: 20 June 2024
Special Issue in
Cancers
Correlating Patient-Reported Quality of Life before, during, and after Therapy with Objective Measures and Outcomes
Guest Editors: Anurag K. Singh, Evan Michael GraboyesDeadline: 5 July 2024
Topical Collections
Topical Collection in
Cancers
Drug Resistance and Novel Therapies in Cancers
Collection Editor: Zhixiang Wang










