2017 ASH:Venetoclax在复发或难治性del17p突变慢性淋巴细胞白血病临床实践中的效果评估
2017-12-06 MedSci MedSci原创
BCL2抑制剂Venetoclax现已批准用于复发或难治性del17p突变慢性淋巴细胞白血病并且对激酶抑制剂治疗失败的患者也具有良好的效果。近日研究人员对204名接受Venetoclax治疗的患者资料进行了考察,以分析Venetoclax在临床实践过程中的效果、毒副作用以及用药剂量情况。研究人员对美国20个临床中心的接受Venetoclax治疗的CLL患者资料进行回顾性队列研究,考察人口统计学、临

BCL2抑制剂Venetoclax现已批准用于复发或难治性del17p突变慢性淋巴细胞白血病并且对激酶抑制剂治疗失败的患者也具有良好的效果。近日研究人员对204名接受Venetoclax治疗的患者资料进行了考察,以分析Venetoclax在临床实践过程中的效果、毒副作用以及用药剂量情况。
研究人员对美国20个临床中心的接受Venetoclax治疗的CLL患者资料进行回顾性队列研究,考察人口统计学、临床及遗传预后因素,Venetoclax剂量升级、肿瘤溶解综合征(TLS)防治、不良事件(AE)、总缓解率(ORR)、完全缓解(CR)、预后以及Venetoclax停药情况。研究的主要终点为无进展生存。
204名CLL患者参与研究,治疗起始平均年龄67岁,男性占70%,白人占89%,73%的患者Rai分级大于2,平均接受过3次其他治疗,del17p+占44%,del11q+占28%,TP53突变占41%,33% 的患者存在复合突变。此外,NOTCH1突变率为27%,BTK突变率为27% ,PLCγ2突变率为10%,IGHV野生型为81%。在Venetoclax治疗前,64%的患者接受了激酶抑制剂治疗,15%的患者接受过2种以上激酶抑制剂治疗,5.4%的患者接受了细胞疗法,4%的患者使用过2代激酶抑制剂,4%的患者使用过其他BCL-2抑制剂。患者最后一次治疗到开始Venetoclax疗法的平均时间为2个月。为应对TLS,93% 的患者使用了别嘌呤醇,92% 的患者使用生理盐水,45%的患者使用了拉布立酶,83%的患者进行了超过1次的住院监测。用药过程中,84%的患者剂量递增到每日400mg的最大推荐剂量。26%的患者出现停药,平均停药时间2天。不良事件包括嗜中性白细胞减少症(48%)、血小板减少(27%)、腹泻(14%)以及中性粒细胞减少性发热(9.4%)。治疗的总响应率为77%,其中完全缓解率为28%,平均最大响应时间3个月。对于BTK或 PLCγ2突变患者,总响应率为90%,完全缓解率为14%。平均随访10个月中,35%的患者终止治疗,未达到主要终点。最常见的治疗终止因素为CLL进展(47%)、Richter综合征(21%)以及治疗毒性(11%,主要为血液毒性)。Venetoclax疗法前因素及遗传因素会降低Venetoclax的治疗效果,导致无进展生存率降低,包括:激酶疗法(HR,3.7)、细胞疗法(HR,4.6)、TP53突变(HR,2.8)、多突变因素(HR,1.9)。Venetoclax治疗失败后,最常见的后续疗法包括激酶抑制剂(47.6%, n=19)、利妥昔单抗(12.5%, n=5)以及细胞疗法(12.5%, n=5),其中激酶抑制剂后续疗法患者的总响应率为69%,无进展生存未达到终点。
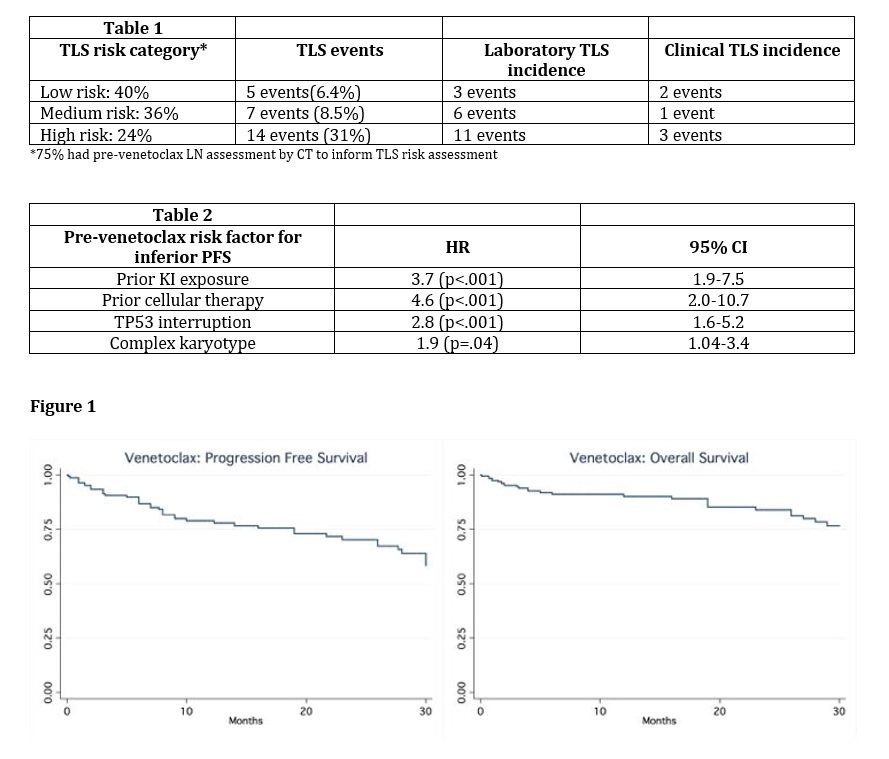
研究发现,在Venetoclax临床实践中,大多数患者实现并保持每日400mg的最大剂量。总响应率以及完全缓解率与临床试验过程相近。Venetoclax对伊布替尼耐药患者有效,之前接受过激酶抑制剂以及存在特殊基因突变的患者会导致无进展生存期缩短。血液毒性是最常见的不良事件,疾病进展是最常见的治疗终止因素。住院监控和拉布立酶常用于肿瘤溶解综合征的预防。激酶抑制剂最常用于Venetoclax的后续治疗,但效果并不显著。
原文链接:
本网站所有内容来源注明为“梅斯医学”或“MedSci原创”的文字、图片和音视频资料,版权均属于梅斯医学所有。非经授权,任何媒体、网站或个人不得转载,授权转载时须注明来源为“梅斯医学”。其它来源的文章系转载文章,或“梅斯号”自媒体发布的文章,仅系出于传递更多信息之目的,本站仅负责审核内容合规,其内容不代表本站立场,本站不负责内容的准确性和版权。如果存在侵权、或不希望被转载的媒体或个人可与我们联系,我们将立即进行删除处理。
在此留言









#淋巴细胞白血病#
31
#NET#
24
#效果评估#
23
#del17p#
30
#ASH#
24
#淋巴细胞#
25
#临床实践#
22
#难治性#
33