Sci Rep:抑郁症改变了大脑的连接
2017-08-13 葛鹏, 董堃 科研圈
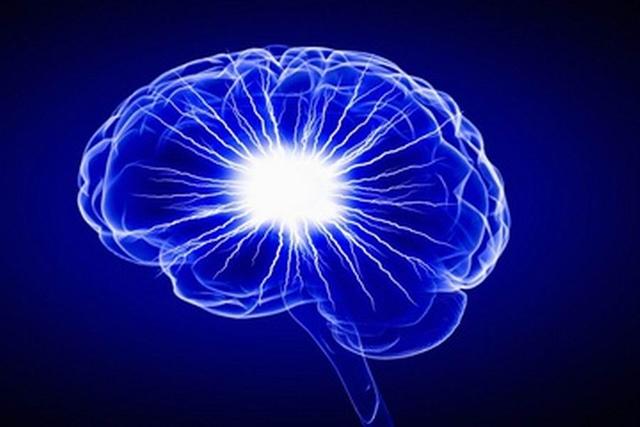
科学家们已经证实抑郁症与脑内白质的结构有关联,白质区域负责连接灰质,确保我们能恰如其分地处理情绪与想法。
本网站所有内容来源注明为“梅斯医学”或“MedSci原创”的文字、图片和音视频资料,版权均属于梅斯医学所有。非经授权,任何媒体、网站或个人不得转载,授权转载时须注明来源为“梅斯医学”。其它来源的文章系转载文章,或“梅斯号”自媒体发布的文章,仅系出于传递更多信息之目的,本站仅负责审核内容合规,其内容不代表本站立场,本站不负责内容的准确性和版权。如果存在侵权、或不希望被转载的媒体或个人可与我们联系,我们将立即进行删除处理。
在此留言











这样大样本量的功能磁共振研究真是难得!
73
???!!!!!!!!!!?!…
73
学习
62
很好,不错,以后会多学习
65
不错的文章,值得推荐
54
已经证实抑郁症与脑内白质的结构有关联
28
TMS是否能作为潜在的治疗方案?
23
学习谢谢分享
29
学习了谢谢分享
24
学习了,学习了
37