常见消化道瘘的影像学表现--直肠-阴道瘘
2015-02-03 首都医科大学附属北京朝阳医院 蒋涛 中国医学论坛报
直肠阴道瘘是指直肠前壁和阴道后壁之间形成的病理性通道,常见病因包括产伤、炎性肠病、手术创伤、感染(直肠周围、盆腔脓肿、憩室炎、前庭大腺炎、盆底炎性疾病)、盆底新生物和盆底放疗(主要是宫颈癌放疗)后等,不常见原因包括硬化剂内痔注射后、直肠阴道损伤、放射性阴道纤维化行扩张治疗后、吻合器痔上黏膜环切术后等。 MRI是显示直肠阴道瘘的主要影像学检查手段,除显示瘘管本身外,对于形成直肠阴道瘘的原因
直肠阴道瘘是指直肠前壁和阴道后壁之间形成的病理性通道,常见病因包括产伤、炎性肠病、手术创伤、感染(直肠周围、盆腔脓肿、憩室炎、前庭大腺炎、盆底炎性疾病)、盆底新生物和盆底放疗(主要是宫颈癌放疗)后等,不常见原因包括硬化剂内痔注射后、直肠阴道损伤、放射性阴道纤维化行扩张治疗后、吻合器痔上黏膜环切术后等。
MRI是显示直肠阴道瘘的主要影像学检查手段,除显示瘘管本身外,对于形成直肠阴道瘘的原因如恶性肿瘤、局部炎症改变及放疗相关的纤维化和组织粘连等的显示效果均较好。
瘘管的MRI表现取决于其内所含成分,T2WI呈高信号(液体)或无信号(气体)或出现气液平面,阴道后壁及直肠前壁肌层信号连续性中断,增强扫描瘘管可出现管道状强化。当然瘘管及瘘口较小时可能会出现假阴性结果。
CT与MRI相比,扫描速度较快,对于不能完成MRI检查的幽闭恐惧患者可以选择CT检查。多层螺旋CT扫描及三维重建技术可以直接显示瘘管,在扫描前口服水溶性造影剂对瘘管的显示更加清晰,同时可以发现阴道及直肠壁瘘口。据报道,阴道造影对于直肠阴道瘘的显示效果优于下消化道造影,可发现多条瘘管和瘘口,同时避免下消化道造影钡剂瘘入盆腔,但现在临床很少用阴道造影。

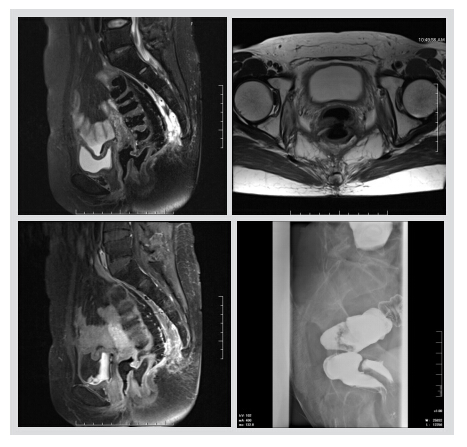
图 患者女性,34岁。直肠阴道瘘。MR矢状位及横断位T2WI及矢状位增强扫描T1WI显示阴道后壁及直肠前壁连续性中断,二者管腔相通-直肠阴道瘘。下消化道造影显示直肠内造影剂进入阴道
本网站所有内容来源注明为“梅斯医学”或“MedSci原创”的文字、图片和音视频资料,版权均属于梅斯医学所有。非经授权,任何媒体、网站或个人不得转载,授权转载时须注明来源为“梅斯医学”。其它来源的文章系转载文章,或“梅斯号”自媒体发布的文章,仅系出于传递更多信息之目的,本站仅负责审核内容合规,其内容不代表本站立场,本站不负责内容的准确性和版权。如果存在侵权、或不希望被转载的媒体或个人可与我们联系,我们将立即进行删除处理。
在此留言







非常好的文章,学习
74
?学习了
107
?学习了
100
#消化道#
18