JACC:极低体重房颤患者的抗凝治疗——DOACs vs 华法林
2019-03-11 不详 MedSci原创
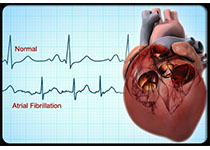
目前,对于非瓣膜性房颤(AF)和极低体重(50kg)患者,直接口服抗凝药物(DOACs)的有效性和安全性尚不清楚。本研究的目的旨在评估和比较DOACs和华法林对极低体重AF患者的效果。本研究纳入了韩国国家数据库中的接受口服抗凝药物治疗的体重≤60kg的AF患者(DOACs n=14013;华法林 n=7576),并用倾向性评分调整两组患者。分析结果显示,与华法林相比,DOACs 与更低的缺血性卒中
本文系梅斯医学(MedSci)原创编译整理,转载需授权!
本网站所有内容来源注明为“梅斯医学”或“MedSci原创”的文字、图片和音视频资料,版权均属于梅斯医学所有。非经授权,任何媒体、网站或个人不得转载,授权转载时须注明来源为“梅斯医学”。其它来源的文章系转载文章,或“梅斯号”自媒体发布的文章,仅系出于传递更多信息之目的,本站仅负责审核内容合规,其内容不代表本站立场,本站不负责内容的准确性和版权。如果存在侵权、或不希望被转载的媒体或个人可与我们联系,我们将立即进行删除处理。
在此留言









#JACC#
0
很好的学习机会
86
很好的学习机会
90
#ACS#
42
#ACC#
42
#DOACs#
31
#房颤患者#
24