JCO:舒尼替尼维持治疗可改善小细胞肺癌无进展生存期PFS(II期研究)
2015-05-04 徐媛媛译 MedSci原创
目的:评估的化疗后使用舒尼替尼治疗小细胞肺癌(SCLC)的有效性。 该试验是一项随机、安慰剂对照、二期试验。将收纳的患者按1:1被随机分配到对照组或舒尼替尼治疗组并进行每天37.5mg直到有进展。交叉后进展是允许的。 本研究一共收纳了144名患者,其中,138名患者接受化疗,95名患者被随机分分配到对照组,10名患者没有接受维持治疗。85名患者接收了维持治疗(对照组组41名;舒尼替尼组
目的:评估的化疗后使用舒尼替尼治疗小细胞肺癌(SCLC)的有效性。
该试验是一项随机、安慰剂对照、二期试验。将收纳的患者按1:1被随机分配到对照组或舒尼替尼治疗组并进行每天37.5mg直到有进展。交叉后进展是允许的。
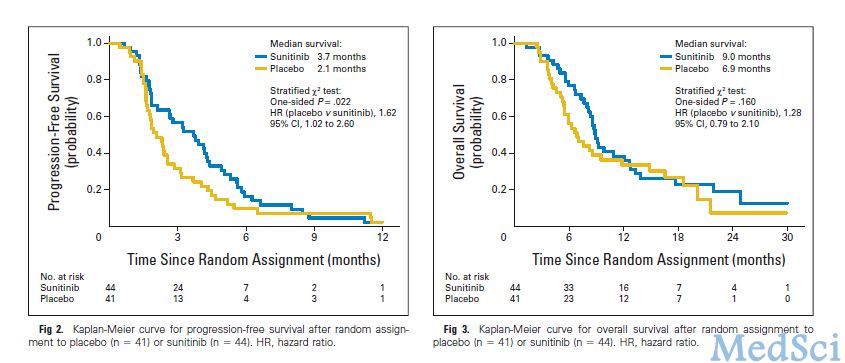
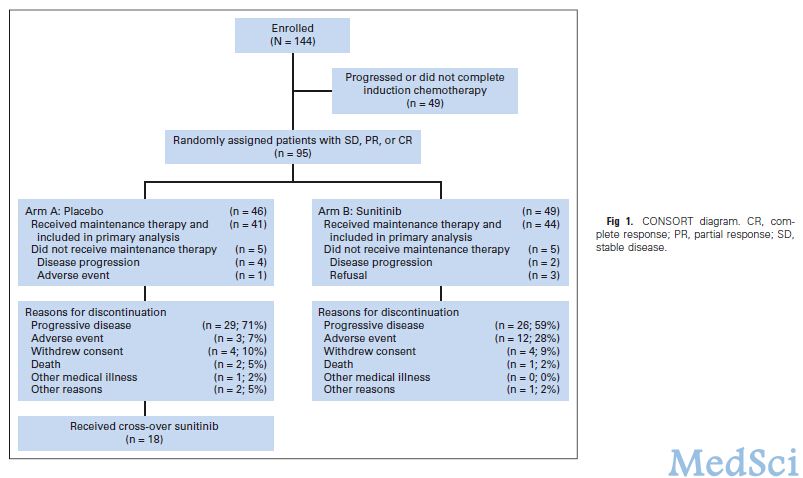
本研究一共收纳了144名患者,其中,138名患者接受化疗,95名患者被随机分分配到对照组,10名患者没有接受维持治疗。85名患者接收了维持治疗(对照组组41名;舒尼替尼组44名)。在舒尼替尼组中,3级不良事件包括疲劳(19%),中性粒细胞减少(7%),白细胞减少(7%),和血小板减少(7%)。在安慰剂组中,只有疲劳(10%)发生在超过5%的队列中。在舒尼替尼组中,4级不良事件包括1例患者出现级消化道出血,1例出现胰腺炎,低血钙,和脂肪酶升高。在安慰剂组中,血小板减少症有1例患者,高钠血症出现1例。对照组中位PFS是3.7个月,舒尼替尼组中位PFS为2.1个月(HR, 1.62; 70% CI, 1.27 to 2.08; 95% CI, 1.02 to 2.60; one-sided P = .02)。中位总生存期,安慰剂组是6.9个月,舒尼替尼组是9个月(HR, 1.28; 95% CI, 0.79 to 2.10; one-sided P = .16)。在舒尼替尼组维持治疗过程中,有三例患者得到缓解。在对照组的13名患者中有10名(77%)患者在进展后转至舒尼替尼治疗被评估为病情稳定(6~27周)。
结论:舒尼替尼维持治疗具有安全以及改善小细胞肺癌无进展生存期(PFS)。
原始出处
Ready NE1, Pang HH2, Gu L2, Otterson GA2, Thomas SP2, Miller AA2, Baggstrom M2, Masters GA2, Graziano SL2, Crawford J2, Bogart J2, Vokes EE2.Chemotherapy With or Without Maintenance Sunitinib for Untreated Extensive-Stage Small-Cell Lung Cancer: A Randomized, Double-Blind, Placebo-Controlled Phase II Study-CALGB 30504 (Alliance).J Clin Oncol. 2015 Mar 2.
本网站所有内容来源注明为“梅斯医学”或“MedSci原创”的文字、图片和音视频资料,版权均属于梅斯医学所有。非经授权,任何媒体、网站或个人不得转载,授权转载时须注明来源为“梅斯医学”。其它来源的文章系转载文章,或“梅斯号”自媒体发布的文章,仅系出于传递更多信息之目的,本站仅负责审核内容合规,其内容不代表本站立场,本站不负责内容的准确性和版权。如果存在侵权、或不希望被转载的媒体或个人可与我们联系,我们将立即进行删除处理。
在此留言









#JCO#
28
#生存期#
18
#PFS#
21
#无进展生存期#
0