冠脉造影正常,凭什么说心梗?
2018-01-30 黄一林 医学界心血管频道
心梗的主要病因在冠状动脉粥样硬化病变的基础上,不稳定斑块破裂诱发血栓堵塞血管所致。但还有10%~15%的心梗发生在冠状动脉造影无明显异常及一些非动脉粥样硬化性疾病的患者。
本网站所有内容来源注明为“梅斯医学”或“MedSci原创”的文字、图片和音视频资料,版权均属于梅斯医学所有。非经授权,任何媒体、网站或个人不得转载,授权转载时须注明来源为“梅斯医学”。其它来源的文章系转载文章,或“梅斯号”自媒体发布的文章,仅系出于传递更多信息之目的,本站仅负责审核内容合规,其内容不代表本站立场,本站不负责内容的准确性和版权。如果存在侵权、或不希望被转载的媒体或个人可与我们联系,我们将立即进行删除处理。
在此留言
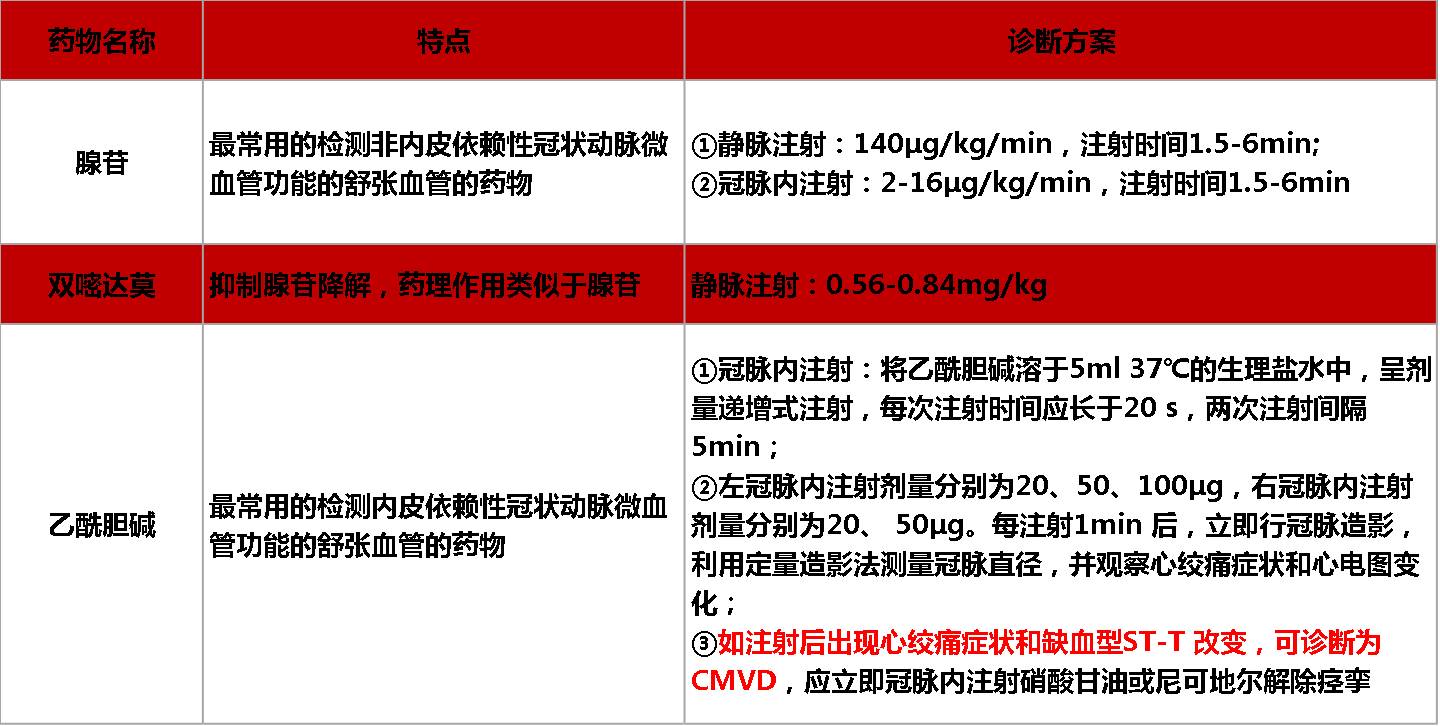




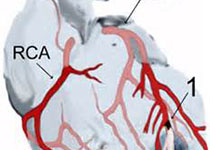





诊断越来越依赖于仪器.必然会产生类似的疑问.
73
学习一下谢谢分享
70
学习谢谢分享!
67
#造影#
26
#冠脉造影#
55
学习了.谢谢分享
61
阅
61
涨见识了.谢谢分享
22
很详细.非常好.谢谢
19
学习了谢谢了
25