JAMA Surg:淋巴结转移阴性食管腺癌患者无需新辅助放化疗
2015-11-15 MedSci MedSci原创
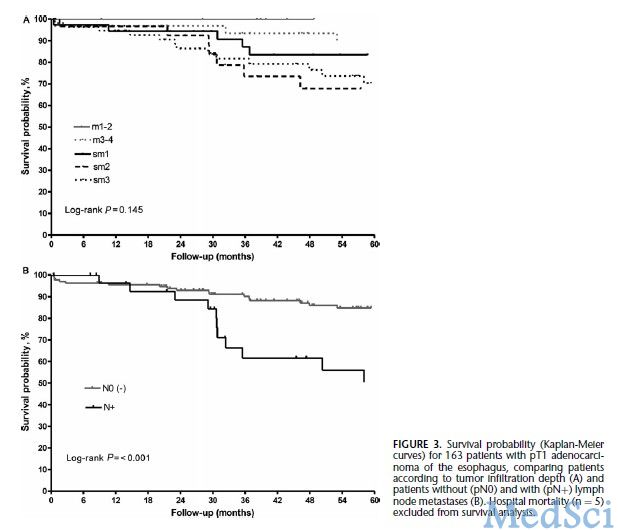
cN+食管腺癌患者显著受益于新辅助放化疗。然而,cN−肿瘤患者新辅助放化疗加手术治疗与单独手术相比总体生存率没有显著改善。这一发现可能对cN−患者使用新辅助放化疗产生重大影响。
本网站所有内容来源注明为“梅斯医学”或“MedSci原创”的文字、图片和音视频资料,版权均属于梅斯医学所有。非经授权,任何媒体、网站或个人不得转载,授权转载时须注明来源为“梅斯医学”。其它来源的文章系转载文章,或“梅斯号”自媒体发布的文章,仅系出于传递更多信息之目的,本站仅负责审核内容合规,其内容不代表本站立场,本站不负责内容的准确性和版权。如果存在侵权、或不希望被转载的媒体或个人可与我们联系,我们将立即进行删除处理。
在此留言








#食管腺#
31
#新辅助#
24
#辅助放化疗#
20
#放化疗#
26
#淋巴结#
35
#淋巴结转移#
28
#新辅助放化疗#
25
#食管#
20
#食管腺癌#
29
难说
130