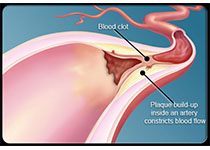
Blood:创伤性脑损伤会释放血管性血友病因子(VWF),进而增强微泡诱导性血管渗液和凝血紊乱
2018-06-26 MedSci MedSci原创
中心点:受伤的大脑会释放超粘连的、与微泡结合的VWF,引发神经功能障碍和全身高凝状态。ADAMTS-13可保护血脑屏障,预防TBI诱导的神经功能障碍和全身性凝血紊乱。摘要:血管性血友病因子(VWF)是一种粘连性配体,活性受金属蛋白酶ADAMTS-13调控。现广泛认为血浆VWF水平升高是创伤和炎症中内皮细胞激活的标志,但其潜在病理机制尚不明确。现有研究人员通过流体打击受损小鼠模型发现急性创伤性脑损伤
受伤的大脑会释放超粘连的、与微泡结合的VWF,引发神经功能障碍和全身高凝状态。
ADAMTS-13可保护血脑屏障,预防TBI诱导的神经功能障碍和全身性凝血紊乱。
摘要:
血管性血友病因子(VWF)是一种粘连性配体,活性受金属蛋白酶ADAMTS-13调控。现广泛认为血浆VWF水平升高是创伤和炎症中内皮细胞激活的标志,但其潜在病理机制尚不明确。
现有研究人员通过流体打击受损小鼠模型发现急性创伤性脑损伤(TBI)可激活VWF释放、形成VWF微泡。VWF微泡可促进全身血管渗液、凝血。在TBI前或后给予重组ADAMTS-13可降低VWF活性,但基本不影响VWF分泌。
rADAMTS-13可通过增强VWF的清除保护内皮细胞屏障的完整性、预防TBI诱导的凝血紊乱,并且不影响基础稳态。用乳凝集素促进微泡清除的效果与rADAMTS-13类似。
本研究揭示了VWF和细胞微泡在TBI诱导性血管渗液和凝血紊乱中发挥协同作用,证实rADAMTS-13对TBI诱导性凝血紊乱具有保护作用。
原始出处:
Yingang Wu, et al.Von Willebrand factor enhanced microvesicle-induced vascular leakage and coagulopathy in mice with traumatic brain injury.Blood 2018 :blood-2018-03-841932; doi: https://doi.org/10.1182/blood-2018-03-841932
本网站所有内容来源注明为“梅斯医学”或“MedSci原创”的文字、图片和音视频资料,版权均属于梅斯医学所有。非经授权,任何媒体、网站或个人不得转载,授权转载时须注明来源为“梅斯医学”。其它来源的文章系转载文章,或“梅斯号”自媒体发布的文章,仅系出于传递更多信息之目的,本站仅负责审核内容合规,其内容不代表本站立场,本站不负责内容的准确性和版权。如果存在侵权、或不希望被转载的媒体或个人可与我们联系,我们将立即进行删除处理。
在此留言









#血管性#
31
#创伤性#
38
#诱导性#
34
#血友病因子#
34
#创伤#
35
#vWF#
38
#损伤#
27
#微泡#
36
学习了.长知识
60